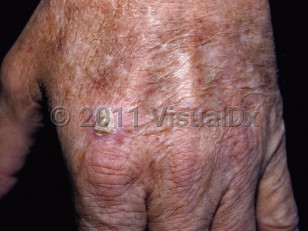
Actinic keratosis
See also in: External and Internal Eye,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

The frequency of AKs increases with age and cumulative lifetime sun exposure. They are also more common in individuals who are immunosuppressed (especially after solid organ transplantation) and in males. They may resolve with protection from ultraviolet (UV) light. Some medications (ie, capecitabine, sorafenib) may induce inflammation of existing AKs.
Patients with AKs are at higher risk for developing nonmelanoma skin cancer. AKs have the potential to evolve into squamous cell carcinoma (SCC). It is estimated that the likelihood that a given AK will evolve into an invasive SCC is approximately 0.075%-0.096% per lesion.
The term "field cancerization" is used to describe areas of skin at risk for both AK and SCC. Clinically, this manifests as numerous AKs and squamous cell carcinoma in situ (SCCis) with or without invasive SCCs in a field of chronically sun-damaged skin. Risk factors include male sex, lighter skin color, older age, underlying immunosuppression, and the degree of prior exposure to UV light.
Related topic: actinic cheilitis
Codes
L57.0 – Actinic keratosis
SNOMEDCT:
201101007 – Actinic keratosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:02/10/2022
 Patient Information for Actinic keratosis
Patient Information for Actinic keratosis - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient