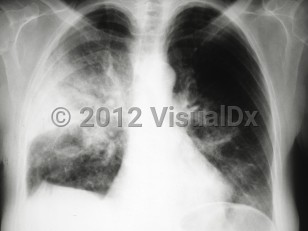
Acute eosinophilic pneumonia
Alerts and Notices
Important News & Links
Synopsis

The primary (intrinsic) form is classically idiopathic, but it is hypothesized that the reaction develops after inhalation of an allergen or irritant. It occurs most often in the setting of initiation or resumption of cigarette smoking, and has been seen with heavy smoke inhalation and inhalation of sand and dust. It can occur at any age but is most common between the ages of 20 and 40, with men being affected twice as frequently as women.
The secondary (extrinsic) form can be a consequence of immune reaction to parasitic or fungal infection, or an adverse reaction to therapeutic or illicit drug use.
Acute eosinophilic pneumonia is associated clinically with the rapid development of hypoxemic respiratory failure, often at presentation, and often requiring mechanical ventilation. Patients present with symptoms of <4 weeks' duration, with nonproductive cough, progressive dyspnea, fever, and sometimes malaise and pleuritic pain. Peripheral eosinophilia is rare in the idiopathic form at presentation but may develop later in the illness. There is no multisystem involvement in the idiopathic form.
Radiographic findings are variable and nonspecific. Ground glass and reticular opacities are often seen on chest x-ray and high-resolution computed tomography (HRCT), as well as small bilateral pleural effusions.
The offending agent should be discontinued if drug-related acute eosinophilic pneumonia is considered. If an infectious etiology is suspected, it should be investigated and treated, and involvement of a specialist in infectious diseases is recommended.
Patients with the idiopathic form of acute eosinophilic pneumonia often have a rapid response to glucocorticoids. Pleural effusions may be slower to resolve than parenchymal opacities.
Codes
J82.82 – Acute eosinophilic pneumonia
SNOMEDCT:
64936001 – Löffler's syndrome
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/06/2017