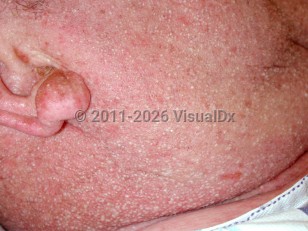
Acute generalized exanthematous pustulosis in Adult
Alerts and Notices
Important News & Links
Synopsis

The syndrome occurs within 2 weeks of starting the inciting medication, usually as soon as 48 hours after initial drug ingestion. Fever, typically up to 39°C (102.2°F), is a near constant feature and persists about 1 week. The rash of AGEP consists of tiny, superficial pustules that develop on erythematous plaques. Burning and pruritus are frequently reported. Lesions resolve within 1-2 weeks with fine, pinpoint areas of desquamation. Mucous membrane involvement occurs in atypical AGEP and its presence portends to worse outcome.
Acute localized exanthematous pustulosis, or ALEP, is a localized variant of AGEP. The clinical presentation and course resemble that of AGEP, but the eruption is often localized to the face, neck or chest, and fever is not a common feature. Localized penile and lower extremity involvement has also been reported.
A severe form of AGEP can be associated with septic shock, presenting with hemodynamic instability and multiorgan dysfunction, including renal failure. Other skin findings, including atypical targetoid lesions, vesicles, and facial edema, have been reported. According to a single tertiary care center, this atypical, severe form of AGEP was found in 22% of patients with AGEP.
The causative drugs in AGEP are primarily antibiotics, typically beta-lactam antibiotics (penicillins, aminopenicillins, cephalosporins) and macrolides (azithromycin), but many other drug culprits have been reported, including norfloxacin, calcium channel blockers (eg, diltiazem, nifedipine), antimalarials, doxycycline, vancomycin, isoniazid, carbamazepine, acetaminophen, quinidine, itraconazole, piperazine, NSAIDs (eg, ibuprofen), metronidazole, and pyrimethamine. ALEP has most frequently been reported following beta-lactam antibiotics but has also been described secondary to other antibiotics and a variety of other medication classes. Severe AGEP with septic shock has been reported with vancomycin, amoxicillin, trimethoprim-sulfamethoxazole, metronidazole, and clindamycin.
Codes
L27.0 – Generalized skin eruption due to drugs and medicaments taken internally
L53.8 – Other specified erythematous conditions
SNOMEDCT:
702617007 – Acute generalized exanthematous pustulosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:04/02/2024