Potentially life-threatening emergency
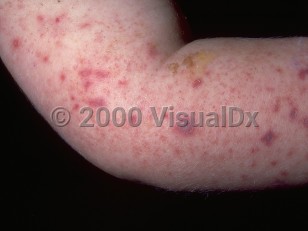
Acute meningococcemia in Adult
Alerts and Notices
Important News & Links
Synopsis

Infection with the gram-negative diplococcus Neisseria meningitidis is responsible for acute meningococcemia, a severe illness that typically occurs in small epidemics. Neisseria meningitidis is transmitted from person to person by respiratory droplets, and the human nasopharynx is the only known reservoir.
The distribution is worldwide, and between 5%-10% of people in the United States are carriers at any given time. Infections are commonly caused by serogroups A, B, C, Y, and W-135 and are more common in crowded areas (such as army barracks and college dormitories), within contacts of infected family members, and in the winter and spring. Males are 3-4 times more susceptible to meningococcemia than females. Increased risk is linked to deficiencies of complement (C5-9), immunoglobulins, and properdin, asplenia, liver disease, systemic lupus erythematosus, enteropathies, and the nephrotic syndrome. Acute meningococcemia has been reported in patients coinfected with HIV and hepatitis C. In the immunocompetent, acute meningococcemia is seen in children younger than 4 years and also in teenagers (and, rarely, in persons of all ages, especially during epidemics).
The clinical picture of acute meningococcemia consists of headache, nausea, vomiting, and severe myalgias that quickly lead to obtundation and a septic-appearing patient. Patients may report a preceding upper respiratory tract infection. Petechiae are the most common cutaneous sign, seen in one-third to one-half of affected patients. Altered mental status, nuchal rigidity, seizures, and gait disturbance can also occur. In asplenic patients, fulminant meningococcemia can lead to sepsis, hypotension, shock, and death in a matter of hours. Complications of acute meningococcemia include pericarditis / myocarditis, disseminated intravascular coagulation (DIC), meningitis and permanent neurologic sequelae, septic arthritis, osteomyelitis, adrenal hemorrhage (Waterhouse-Friderichsen syndrome), gangrene, and death. The overall mortality rate is between 5%-10%; however, meningococcemia associated with DIC has a mortality rate exceeding 90%.
Chronic meningococcemia is characterized by a persistent low fever, rash, and arthralgias, and it is commonly mistaken for gonococcemia.
The distribution is worldwide, and between 5%-10% of people in the United States are carriers at any given time. Infections are commonly caused by serogroups A, B, C, Y, and W-135 and are more common in crowded areas (such as army barracks and college dormitories), within contacts of infected family members, and in the winter and spring. Males are 3-4 times more susceptible to meningococcemia than females. Increased risk is linked to deficiencies of complement (C5-9), immunoglobulins, and properdin, asplenia, liver disease, systemic lupus erythematosus, enteropathies, and the nephrotic syndrome. Acute meningococcemia has been reported in patients coinfected with HIV and hepatitis C. In the immunocompetent, acute meningococcemia is seen in children younger than 4 years and also in teenagers (and, rarely, in persons of all ages, especially during epidemics).
The clinical picture of acute meningococcemia consists of headache, nausea, vomiting, and severe myalgias that quickly lead to obtundation and a septic-appearing patient. Patients may report a preceding upper respiratory tract infection. Petechiae are the most common cutaneous sign, seen in one-third to one-half of affected patients. Altered mental status, nuchal rigidity, seizures, and gait disturbance can also occur. In asplenic patients, fulminant meningococcemia can lead to sepsis, hypotension, shock, and death in a matter of hours. Complications of acute meningococcemia include pericarditis / myocarditis, disseminated intravascular coagulation (DIC), meningitis and permanent neurologic sequelae, septic arthritis, osteomyelitis, adrenal hemorrhage (Waterhouse-Friderichsen syndrome), gangrene, and death. The overall mortality rate is between 5%-10%; however, meningococcemia associated with DIC has a mortality rate exceeding 90%.
Chronic meningococcemia is characterized by a persistent low fever, rash, and arthralgias, and it is commonly mistaken for gonococcemia.
Codes
ICD10CM:
A39.2 – Acute meningococcemia
SNOMEDCT:
186365005 – Acute meningococcemia
A39.2 – Acute meningococcemia
SNOMEDCT:
186365005 – Acute meningococcemia
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:04/09/2017
Last Updated:02/17/2020
Last Updated:02/17/2020