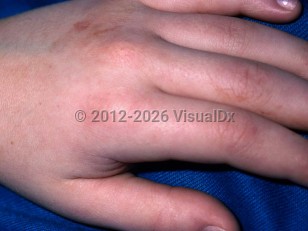
Angioedema - Cellulitis DDx
See also in: Overview,External and Internal Eye,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Angioedema can be caused by medications, foods, or be idiopathic. Drug-induced angioedema can be associated with urticaria, but it can occur alone with deeper tissue swelling being the only manifestation. Angiotensin-converting enzyme (ACE) inhibitors, widely used antihypertensive medications, are a common cause, with angioedema occurring even a year after therapy was initiated. Americans of African descent have 4-5 times greater incidence of ACE inhibitor-induced angioedema than Americans of Northern European descent. ACE inhibitor-induced angioedema often involves the upper airways and can produce a life-threatening risk of respiratory compromise. Other risk factors include female sex, atopy, and cigarette smoking. Other implicated medications include aspirin and other NSAIDs, antibiotics, radiocontrast agents, fibrinolytic agents, and estrogens, including oral contraceptives.
Angioedema as seen in the heritable angioedema syndrome is not responsive to standard antihistamine therapy and usually will not have associated urticaria. Familial forms begin in adolescence; they have autosomal dominant inheritance and are related to disorders of complement regulation. Episodes of angioedema are often precipitated by surgery or accidents.
Acquired C1 esterase inhibitor deficiency also presents with angioedema. It is typically the result of a lymphoproliferative disorder (type 1) or autoimmune disease (type 2). It may result from the formation of autoantibodies against C1 esterase inhibitor or persistent low-level activation of C1q by anti-idiotypic antibodies in patients with B-cell lymphoproliferative disorders.
Tick bites from some Amblyomma and Ixodes (and possibly Haemaphysalis) species have been associated with the subsequent development of allergies to mammalian meat (eg, beef, pork) in a small number of patients (see alpha-gal syndrome). It is thought that the allergy is mediated by induced immunoglobulin E (IgE) antibodies to alpha-gal (galactose-alpha-1,3-galactose), a mammalian oligosaccharide. Individuals with elevated IgE titers to alpha-gal have experienced urticaria, angioedema, and anaphylaxis symptoms either immediately or 3-6 hours (delayed onset) after ingesting mammalian meat. Exactly how the tick bite leads to development of this allergy is unclear.
Idiopathic angioedema is 3 or more episodes of recurrent angioedema with no apparent cause after comprehensive medical evaluation.
The swelling of angioedema is often more marked than that of cellulitis. Conversely, erythema is a less prominent feature. Unlike cellulitis, angioedema almost always occurs bilaterally. In angioedema, there may also be a history of exposure to a known inciting factor.
Codes
T78.3XXA – Angioneurotic edema, initial encounter
SNOMEDCT:
41291007 – Angioedema
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:08/11/2024
 Patient Information for Angioedema - Cellulitis DDx
Patient Information for Angioedema - Cellulitis DDx- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient