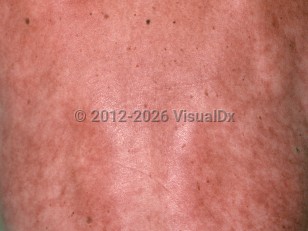
Angioendotheliomatosis
Alerts and Notices
Important News & Links
Synopsis

Angioendotheliomatosis is a cutaneous vascular proliferation of endothelial cells within blood vessels. It includes benign and malignant forms.
Reactive angioendotheliomatosis (RAE):
Benign angioendotheliomatosis, also known as reactive angioendotheliomatosis (RAE), is a rare self-limited condition that can occur at any age. Most cases are idiopathic; however, RAE has been known to occur in association with numerous systemic diseases that may cause inflammation or obliteration of the vascular lumina. Such diseases include autoimmune conditions (eg, systemic lupus erythematosus), subacute bacterial endocarditis, cryoglobulinemia, hepatic disease, monoclonal gammopathy (eg, monoclonal gammopathy of undetermined significance), chronic lymphocytic leukemia, renal disease, rheumatoid arthritis, antiphospholipid antibody syndrome, and atherosclerotic disease. It has also been observed in the setting of trauma. RAE is hypothesized to occur in response to a circulating capillary growth factor or perhaps a growth factor released in response to tissue hypoxia. In addition to the skin findings of erythematous papules and plaques, there may be constitutional symptoms such as fever, chills, malaise, and weight loss with this disorder.
Angiotropic lymphoma:
What was historically referred to as malignant angioendotheliomatosis is now more properly known as intravascular large cell lymphoma or angiotropic lymphoma. The misnomer angioendotheliomatosis stems from the fact that this condition is characterized by an intraluminal proliferation of large, atypical cells that were thought to be derived from endothelial cells. Advances in immunohistochemistry demonstrated that these neoplastic cells are of lymphoid origin, and while cases of T-cell origin have been reported, the most recent literature supports that the majority of cases are B-cell proliferations. There is a slight tendency toward increased incidence among males, and the average age of presentation is 70 years. Precise incidence is uncertain, as most of the literature on this condition has been in the form of case reports and small case series. This condition is aggressive and rapidly fatal.
Angiotropic lymphoma most commonly presents with fever and central nervous system (CNS) symptoms. Because of the vague presenting symptoms and the rapid course, about half of reported cases are diagnosed only on autopsy. Patients often have an elevated serum lactate dehydrogenase (LDH) and ESR, anemia, thrombocytopenia, and leukopenia.
About 26% of patients present with only cutaneous symptoms. This variant is almost exclusively seen in women with an average age of presentation of 59 years. Most patients present with disseminated and advanced disease. Additionally, an Asian variant has been described that occurs predominantly but not exclusively in Japan and is characterized by multi-organ failure, hepatosplenomegaly, pancytopenia, and hemophagocytic syndrome.
Cases arising in the setting of other malignancies have been reported. Although the precise incidence is unknown, 1 series of 38 patients found 16% had either a history of or a concomitant distinct malignancy. This includes both hematopoietic and solid tumors. Approximately one-third of these cases represent non-Hodgkin lymphomas, with diffuse large B-cell lymphomas being the most common. Cases of small lymphocytic lymphomas, follicular lymphomas, and mucosa-associated lymphoid tissue lymphomas have been reported.
There are no known risk factors for angioendotheliomatosis.
Reactive angioendotheliomatosis (RAE):
Benign angioendotheliomatosis, also known as reactive angioendotheliomatosis (RAE), is a rare self-limited condition that can occur at any age. Most cases are idiopathic; however, RAE has been known to occur in association with numerous systemic diseases that may cause inflammation or obliteration of the vascular lumina. Such diseases include autoimmune conditions (eg, systemic lupus erythematosus), subacute bacterial endocarditis, cryoglobulinemia, hepatic disease, monoclonal gammopathy (eg, monoclonal gammopathy of undetermined significance), chronic lymphocytic leukemia, renal disease, rheumatoid arthritis, antiphospholipid antibody syndrome, and atherosclerotic disease. It has also been observed in the setting of trauma. RAE is hypothesized to occur in response to a circulating capillary growth factor or perhaps a growth factor released in response to tissue hypoxia. In addition to the skin findings of erythematous papules and plaques, there may be constitutional symptoms such as fever, chills, malaise, and weight loss with this disorder.
Angiotropic lymphoma:
What was historically referred to as malignant angioendotheliomatosis is now more properly known as intravascular large cell lymphoma or angiotropic lymphoma. The misnomer angioendotheliomatosis stems from the fact that this condition is characterized by an intraluminal proliferation of large, atypical cells that were thought to be derived from endothelial cells. Advances in immunohistochemistry demonstrated that these neoplastic cells are of lymphoid origin, and while cases of T-cell origin have been reported, the most recent literature supports that the majority of cases are B-cell proliferations. There is a slight tendency toward increased incidence among males, and the average age of presentation is 70 years. Precise incidence is uncertain, as most of the literature on this condition has been in the form of case reports and small case series. This condition is aggressive and rapidly fatal.
Angiotropic lymphoma most commonly presents with fever and central nervous system (CNS) symptoms. Because of the vague presenting symptoms and the rapid course, about half of reported cases are diagnosed only on autopsy. Patients often have an elevated serum lactate dehydrogenase (LDH) and ESR, anemia, thrombocytopenia, and leukopenia.
About 26% of patients present with only cutaneous symptoms. This variant is almost exclusively seen in women with an average age of presentation of 59 years. Most patients present with disseminated and advanced disease. Additionally, an Asian variant has been described that occurs predominantly but not exclusively in Japan and is characterized by multi-organ failure, hepatosplenomegaly, pancytopenia, and hemophagocytic syndrome.
Cases arising in the setting of other malignancies have been reported. Although the precise incidence is unknown, 1 series of 38 patients found 16% had either a history of or a concomitant distinct malignancy. This includes both hematopoietic and solid tumors. Approximately one-third of these cases represent non-Hodgkin lymphomas, with diffuse large B-cell lymphomas being the most common. Cases of small lymphocytic lymphomas, follicular lymphomas, and mucosa-associated lymphoid tissue lymphomas have been reported.
There are no known risk factors for angioendotheliomatosis.
Codes
ICD10CM:
C83.30 – Diffuse large B-cell lymphoma, unspecified site
C85.80 – Other specified types of non-Hodgkin lymphoma, unspecified site
SNOMEDCT:
1157162007 – Intravascular large B-cell lymphoma
C83.30 – Diffuse large B-cell lymphoma, unspecified site
C85.80 – Other specified types of non-Hodgkin lymphoma, unspecified site
SNOMEDCT:
1157162007 – Intravascular large B-cell lymphoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:08/20/2023
Last Updated:09/13/2023
Last Updated:09/13/2023
Angioendotheliomatosis