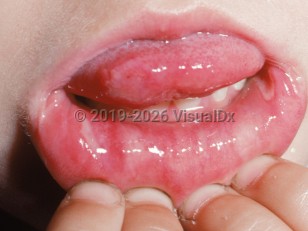
Aphthous ulcers are divided into 3 main subtypes: minor, major, and herpetiform. Minor and major aphthae are the predominant subtypes seen in pediatric patients.
Minor aphthae (Mikulicz ulcers) represent about 87% of pediatric cases and are single or multiple lesions that are 1.0 cm or less in diameter, mildly painful, and which generally heal within 1-2 weeks without scarring. They favor the buccal mucosa, labial mucosa, and the floor of the mouth. They usually develop in childhood or adolescence and continue to occur sporadically throughout life.
Major aphthae (Sutton disease) represent approximately 13% of pediatric cases. They are greater than 1 cm in diameter and are usually first seen at the onset of puberty. These lesions are extremely painful, last from 2-6 weeks, and generally heal with scarring. They favor the labial mucosa, soft palate, tongue, or pharynx. Systemic symptoms, such as fever and odynophagia, may be seen.
Herpetiform aphthae typically do not appear until adulthood. They are characterized by multiple ulcerations that are 1-3 mm in diameter and occur in clusters. Their clinical course is similar to that of minor aphthous ulcers in that they usually heal in less than one month without scarring. They can be seen anywhere on the oral mucosa. They are more common in females.
Most patients with aphthous ulcers suffer recurrences and this is termed recurrent aphthous stomatitis (RAS). RAS is more common in women, in patients younger than 40, in nonsmokers, and in people of higher socioeconomic status. Prevalence seems to be higher in patients of Northern European descent.
There are 2 well-recognized patterns for recurring oral ulcerations:
- Simple aphthosis is primarily marked by minor aphthae that recur intermittently with disease-free intervals of weeks to months. Patients are generally young and healthy, with lesions limited to the mouth and no underlying systemic disease. Patients frequently report a family history of oral ulceration. In addition to presumed genetic risk, epidemiologic studies (and patient reports) support an association between new lesions and oral trauma, chemical irritation, emotional stress, and smoking cessation. Pregnancy and hormonal changes in menses appear to increase risk. Some studies suggest that those who were breast-fed as infants may be at decreased risk. Most affected individuals experience less severe and fewer episodes after 50 years of age.
- Complex aphthosis is marked by the near-constant presence of 3 or more oral and/or genital aphthae. When genital ulcers are involved, complex aphthosis is sometimes called Lipschütz disease. Complex aphthosis usually occurs in the presence of an underlying disease such as human immunodeficiency virus (HIV), gluten-sensitive enteropathy, inflammatory bowel disease, or Behçet disease. By definition, Behçet disease is accompanied by other findings, including genital ulcers, uveitis, and other skin and systemic inflammatory processes. Complex aphthosis is also seen in rarer conditions such as MAGIC syndrome (mouth and genital ulcers, inflamed cartilage), PFAPA syndrome (periodic fever, aphthous stomatitis, pharyngitis, and lymphadenopathy), and cyclical neutropenia (fever approximately every 3 weeks, oral ulcers, neutropenia).



 Patient Information for
Patient Information for