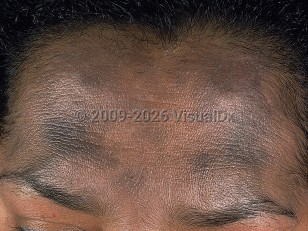
Ashy dermatosis in Adult
Alerts and Notices
Important News & Links
Synopsis

Ashy dermatosis (AD) is an acquired condition of unknown etiology characterized by asymptomatic blue-gray or gray-brown "ashy" macules and/or patches. It is most commonly distributed symmetrically on the neck, trunk, and proximal extremities.
Many consider AD and erythema dyschromicum perstans (EDP) to be synonymous. However, some use the term EDP to refer to the subset of patients who present with annular erythematous / inflammatory borders around the ashy macules and patches, which is usually an early finding.
The umbrella term acquired dermal macular hyperpigmentation (ADMH) has been proposed to encompass AD and other pigmentary disorders with considerable clinical and histological similarities, including lichen planus pigmentosus (LPP), idiopathic eruptive macular hyperpigmentation (IEMH), and pigmented contact dermatitis. These conditions are characterized by dermal hyperpigmentation, lack of a clinically apparent inflammatory phase, and a variably chronic disease course.
Pathogenetically, a cell-mediated immune reaction to antigens located in basal and mid-epidermal keratinocytes is postulated. No definitive cause has been identified; however, AD has been associated with certain exposures, including ammonium nitrate, oral radiographic contrast media, cobalt, enteroviral infection, HIV seroconversion, chronic hepatitis C infection, and whipworm infection. An AD-like eruption from osimertinib and EGFR inhibitors has also been reported. More recently, cutaneous biomarkers involved in regulating melanogenesis have been correlated with phenotypic severity of ADMH disorders. Secreted by fibroblasts, these include Neuregulin 1 (NRG1) and Dickkopf1 (DKK1). NRG1 expression demonstrated a positive correlation with ADMH disease severity, contributing to increased hyperpigmentation, whereas DKK1 expression showed an inverse correlation.
ADMH disorders (including AD) have shown a rising incidence, higher prevalence in females, and a typical onset in middle age, but with cases reported in children as young as age 2 years. AD is most common in individuals with Fitzpatrick skin phototypes III-IV.
Lesions are usually asymptomatic but may be pruritic. Macules often enlarge and coalesce into patches over multiple weeks. Overall, AD is slowly progressive and does not typically regress in adults. In pediatric patients, AD more commonly affects Fitzpatrick I-II skin types and may spontaneously resolve in approximately 50% of cases within 2-3 years.
Many consider AD and erythema dyschromicum perstans (EDP) to be synonymous. However, some use the term EDP to refer to the subset of patients who present with annular erythematous / inflammatory borders around the ashy macules and patches, which is usually an early finding.
The umbrella term acquired dermal macular hyperpigmentation (ADMH) has been proposed to encompass AD and other pigmentary disorders with considerable clinical and histological similarities, including lichen planus pigmentosus (LPP), idiopathic eruptive macular hyperpigmentation (IEMH), and pigmented contact dermatitis. These conditions are characterized by dermal hyperpigmentation, lack of a clinically apparent inflammatory phase, and a variably chronic disease course.
Pathogenetically, a cell-mediated immune reaction to antigens located in basal and mid-epidermal keratinocytes is postulated. No definitive cause has been identified; however, AD has been associated with certain exposures, including ammonium nitrate, oral radiographic contrast media, cobalt, enteroviral infection, HIV seroconversion, chronic hepatitis C infection, and whipworm infection. An AD-like eruption from osimertinib and EGFR inhibitors has also been reported. More recently, cutaneous biomarkers involved in regulating melanogenesis have been correlated with phenotypic severity of ADMH disorders. Secreted by fibroblasts, these include Neuregulin 1 (NRG1) and Dickkopf1 (DKK1). NRG1 expression demonstrated a positive correlation with ADMH disease severity, contributing to increased hyperpigmentation, whereas DKK1 expression showed an inverse correlation.
ADMH disorders (including AD) have shown a rising incidence, higher prevalence in females, and a typical onset in middle age, but with cases reported in children as young as age 2 years. AD is most common in individuals with Fitzpatrick skin phototypes III-IV.
Lesions are usually asymptomatic but may be pruritic. Macules often enlarge and coalesce into patches over multiple weeks. Overall, AD is slowly progressive and does not typically regress in adults. In pediatric patients, AD more commonly affects Fitzpatrick I-II skin types and may spontaneously resolve in approximately 50% of cases within 2-3 years.
Codes
ICD10CM:
L81.8 – Other specified disorders of pigmentation
SNOMEDCT:
58942006 – Erythema dyschromicum perstans
L81.8 – Other specified disorders of pigmentation
SNOMEDCT:
58942006 – Erythema dyschromicum perstans
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:09/11/2025
Last Updated:09/24/2025
Last Updated:09/24/2025
 Patient Information for Ashy dermatosis in Adult
Patient Information for Ashy dermatosis in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Ashy dermatosis in Adult