Most patients with atopic dermatitis experience an early onset, with at least 85% of cases occurring in individuals aged younger than 5 years. Atopic dermatitis morphology and distribution are generally age dependent, with the cheeks, forehead, and scalp as the typical initial areas in infancy. Involvement of extensor surfaces is characteristic of the distribution in infants and young children, while flexural involvement is more characteristic of older children and adolescents.
Atopic dermatitis may be categorized as follows:
- Acute – erythema, vesicles, bullae, weeping, crusting
- Subacute – scaly plaques, papules, round erosions, crusts
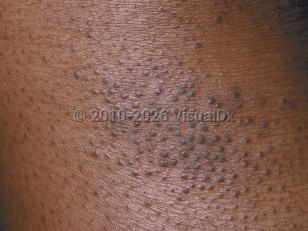
- Chronic eczema – lichenification, scaling, hyper- and hypopigmentation
Intense pruritus is a hallmark of atopic dermatitis. Scratching leads to lichenification (skin thickening). Impaired barrier function results in increased transepidermal water loss and susceptibility to secondary bacterial and viral infections. Patients with atopic dermatitis are prone to impetiginization with Staphylococcus aureus (impetigo). Secondary infections with herpes simplex virus (eczema herpeticum, a medical emergency where early treatment with antiviral therapy is essential), Coxsackie viruses (eczema coxsackium), vaccinia virus (eczema vaccinatum), or molluscum contagiosum may occur.
Patients with atopic dermatitis have difficulties in retaining skin moisture and suffer from xerosis (dry skin). Environmental triggers, such as heat, humidity, detergents / soaps, abrasive clothing, chemicals, smoke, and even stress, tend to aggravate the condition. Latex allergy and nickel allergy occur more often in persons with atopic dermatitis. Additionally, patients with atopic dermatitis have been found to be more likely to have positive patch test results to products commonly found in topical treatments, including cocamidopropyl betaine, wool alcohol / lanolin, and tixocortol pivalate. Furthermore, up to 20%-40% of pediatric patients with moderate-to-severe atopic dermatitis have an immunoglobulin E (IgE)-mediated food allergy, most commonly to milk, eggs, and peanuts.
Atopic dermatitis is increasing in the developed world. In the United States, about 10% of children may be affected by atopic dermatitis, but the majority of these cases are mild. Mild cases may improve in adulthood, although some may retain stigmata of dry or sensitive skin.



 Patient Information for
Patient Information for