During the prior smallpox vaccine era, clinicians did not routinely differentiate between atopic dermatitis and other conditions such as contact dermatitis, seborrheic dermatitis, irritant dermatitis, etc. If all of these conditions were considered a contraindication to smallpox vaccination, possibly 30% to 50% of the American population would be excluded from smallpox vaccination. Therefore, atopic dermatitis must be distinguished from other forms of dermatitis. Atopic dermatitis is 2 to 3 times more prevalent today than when the smallpox vaccine was given in the past.
Atopic dermatitis is a specific condition primarily affecting allergy-prone people. The condition is chronic, relapsing, and pruritic and often associated with allergic rhinitis and/or asthma. Infants and children are most often affected, with 85% of cases appearing in the first year of life, and 95% of cases appearing by 5 years. The condition may persist into, or even arise in, adulthood. Less than 1% of adults are affected by atopic dermatitis. With increased understanding of immunosenescence, atopic dermatitis is increasingly being recognized in the geriatric population.
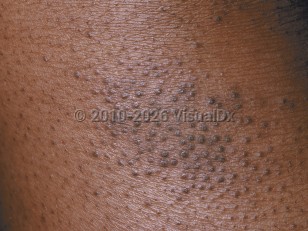
In infants, the disease involves primarily the face, scalp, and torso. In children and adults, the disease usually involves chiefly the flexural aspects of extremities, but it may be more generalized. Follicular patterns of atopic dermatitis (ie, follicular eczema) are more common in persons of color. A lichen planus-like appearance has also been reported in persons of color, due to lichenification and the difficulties in perceiving erythema in darker skin colors.
Atopic dermatitis may be categorized as follows:
- Acute – erythema, vesicles, bullae, weeping, crusting
- Subacute – scaly plaques, papules, round erosions, crusts
- Chronic eczema – lichenification, scaling, hyper- and hypopigmentation
Intense pruritus (itching) is a hallmark of atopic dermatitis. Scratching leads to lichenification (skin thickening). Impaired barrier function leads to increased water loss and cutaneous infections. Patients with atopic dermatitis are prone to impetiginization with Staphylococcus aureus (impetigo). Secondary infections with herpes simplex virus (eczema herpeticum), Coxsackie viruses (eczema coxsackium), or vaccinia virus (eczema vaccinatum) may transpire.
Patients with atopic dermatitis have difficulties in retaining skin moisture and suffer from xerosis (dry skin). Environmental triggers, such as heat, humidity, detergents/soaps, abrasive clothing, chemicals, smoke, and even stress, tend to aggravate the condition. Latex allergy and nickel allergy occur more often in persons with atopic dermatitis. Additionally, patients with atopic dermatitis have been found to be more likely to have positive patch test results to products commonly found in topical treatments, including cocamidopropyl betaine, wool alcohol / lanolin, and tixocortol pivalate. Allergy to eggs, cow's milk, or peanuts is common.



 Patient Information for
Patient Information for