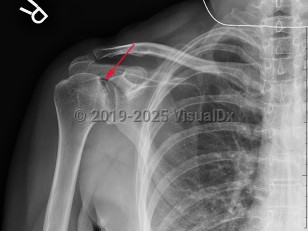
Classic history and presentation: Patients typically present with progressive shoulder pain, stiffness, and weakness without an acute inciting event. This presentation may be secondary to trauma, such as a displaced proximal humerus fracture, or it may be due to atraumatic causes, such as sickle cell anemia or certain medications.
Risk factors: There is an increased risk of avascular necrosis after displaced 3-part and 4-part proximal humerus fractures, with an even higher risk of development with fracture dislocations; these injuries tend to result in a disruption of the blood supply to the bone. Atraumatic risk factors include prolonged corticosteroid use, especially in the setting of systemic lupus erythematosus, homozygous sickle cell disease, alcohol use disorder, decompression illness (Caisson disease), and certain metabolic diseases such as Gaucher disease.
Pathophysiology: The humeral head blood supply is the posterior and anterior circumflex arteries, which can be disrupted by trauma or other conditions that would occlude or disrupt the blood supply.
Grade / classification system: Cruess classification
- Stage 1 – normal x-ray, changes on MRI
- Stage 2 – sclerosis and cystic changes, osteopenia on x-ray
- Stage 3 – crescent sign (subchondral fractures) on x-ray
- Stage 4 – flattening and collapse on x-ray
- Stage 5 – degenerative changes extend to the glenoid on x-ray