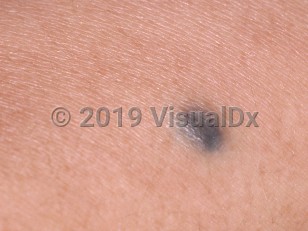
Blue nevus in Adult
See also in: Hair and Scalp,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Blue nevus (also known as a blue mole) is a type of benign acquired nevus. These small blue-gray or blue-black papules represent an aggregate of melanocytes in the upper and mid-dermis. Blue nevi usually develop in young adulthood and are more common in women and in those of Asian descent, although a recent study suggests that onset in adulthood in men is also seen.
Melanocytes originate embryologically in the neural crest and then migrate to the dermal-epidermal junction or to the hair bulb. Blue nevi are hypothesized to arise from melanocytes that fail to complete their developmental journey and instead reside and proliferate in the dermis. Dermal melanocytes reflect low-wavelength blue light but absorb higher wavelength light, a phenomenon known as the Tyndall effect. This accounts for the characteristic blue hue of the lesion. Somatic mutations in GNAQ mutations have recently been found in the majority of blue nevi.
A variant of blue nevus, the cellular blue nevus, is typically larger (1-3 cm in diameter) than a common blue nevus (<1 cm), solitary, and has a predilection for the buttocks or sacrococcygeal region. Malignant blue nevi are rare and tend to arise in cellular blue nevi, especially those on the scalp. Blue nevi are also one of the most common components of combined nevi. Another variant, the epithelioid blue nevus, may be associated with Carney complex (lentigines, atrial myxoma, mucocutaneous myxoma, and nevi).
Related topic: agminated nevus
Melanocytes originate embryologically in the neural crest and then migrate to the dermal-epidermal junction or to the hair bulb. Blue nevi are hypothesized to arise from melanocytes that fail to complete their developmental journey and instead reside and proliferate in the dermis. Dermal melanocytes reflect low-wavelength blue light but absorb higher wavelength light, a phenomenon known as the Tyndall effect. This accounts for the characteristic blue hue of the lesion. Somatic mutations in GNAQ mutations have recently been found in the majority of blue nevi.
A variant of blue nevus, the cellular blue nevus, is typically larger (1-3 cm in diameter) than a common blue nevus (<1 cm), solitary, and has a predilection for the buttocks or sacrococcygeal region. Malignant blue nevi are rare and tend to arise in cellular blue nevi, especially those on the scalp. Blue nevi are also one of the most common components of combined nevi. Another variant, the epithelioid blue nevus, may be associated with Carney complex (lentigines, atrial myxoma, mucocutaneous myxoma, and nevi).
Related topic: agminated nevus
Codes
ICD10CM:
D22.9 – Melanocytic nevi, unspecified
SNOMEDCT:
254806009 – Blue nevus of skin
D22.9 – Melanocytic nevi, unspecified
SNOMEDCT:
254806009 – Blue nevus of skin
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:06/02/2021
 Patient Information for Blue nevus in Adult
Patient Information for Blue nevus in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Blue nevus in Adult
See also in: Hair and Scalp,Oral Mucosal Lesion