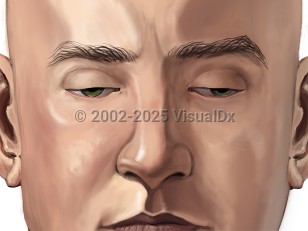
Botulism
Alerts and Notices
Important News & Links
Synopsis

Botulism is caused by a group of paralytic neurotoxins produced by the spore-forming anaerobic gram-positive bacillus Clostridium botulinum. Botulinum toxin irreversibly binds to the pre-synaptic cholinergic neuromuscular junction, blocking acetylcholine release and manifesting as a symmetric progressive descending flaccid paralysis with bulbar palsies after an 18- to 72-hour incubation period. Multiple cranial nerve palsies are evident early in the course of the disease. Symptom severity ranges from mild to frank paralysis. Botulism has a mortality rate of 5%-10% (up to 30% in victims over 60 years of age).
Intoxication can occur naturally from contaminated foods or rarely as a result of wound or intestinal colonization in humans. Rarely, there have been reports of harmful reactions after injections of counterfeit or mishandled (not following state / local requirements) botulinum toxin (commonly called "Botox") for cosmetic or other treatments.
There are 7 types of botulinum toxins, A through G, although only A, B, E, and F have been implicated in the poisoning of humans. Botulinum toxins are odorless and colorless in solution. Botulism is not spread person to person.
People at higher risk for contracting food-borne botulism are nursing home residents, dormitory residents, wedding guests, and large event attendees. Intestinal botulism occurs in infants, and wound botulism must be suspected in IV drug users, particularly black tar heroin users, who present with weakness (in addition to cerebral infection or epidural abscess).
In food-acquired cases, nausea, vomiting, and diarrhea may precede the paralysis, and cases will cluster around consumption of the contaminated food at a restaurant or from improper home canning.
Patients are afebrile with initial complaints of blurred vision, diplopia, and mydriasis with photophobia, ptosis, ophthalmoplegia, hoarseness, dysarthric speech, and dysphagia. Constipation, dry mouth, and urinary retention may also occur. Patients remain awake, alert, and oriented throughout the entire illness. Symptoms progress in a descending pattern to produce a skeletal muscle paralysis that may cause sudden respiratory arrest and death if untreated. Severe poisonings may require months of ventilatory support.
If you have high suspicion for botulism, it is imperative to notify public health officials immediately. They will assist with gauging the likelihood of disease and are the only group who can release the antidote (an antitoxin). Best available data suggests that antitoxin, when administered early, is associated with better clinical outcomes. Antitoxin is available from the US Centers for Disease Control and Prevention (CDC).
Botulinum Toxin and Bioterrorism
Botulism is classified as a Category A bioterrorism agent because of its ease of dissemination and high mortality rate. When used as a biological weapon, botulinum toxin is most likely to be dispersed as an aerosol for inhalation, although it could be added to the food or water supply. Following an aerosol release, the toxin may be swallowed as well as inhaled.
Codes
A05.1 – Botulism food poisoning
SNOMEDCT:
398565003 – Botulism
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
 Patient Information for Botulism
Patient Information for Botulism - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient