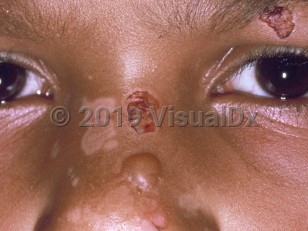
Bullous pemphigoid of childhood in Child
Alerts and Notices
Important News & Links
Synopsis

This summary discusses pediatric patients. Bullous pemphigoid in adults is addressed separately.
Bullous pemphigoid is a chronic autoimmune subepidermal vesiculobullous disease that is most common in older adults. It is rarely seen in infants and children, in whom the precise incidence is unknown.
In the pediatric population, clinical presentation of bullous pemphigoid is variable, with ill-appearing patients who have severe, generalized blisters on one end of the spectrum and patients with localized, asymptomatic lesions on the other. As in adults, pruritic urticarial papules and plaques may precede the formation of bullae. Bullae can be widespread or localized on any body surface. In infants, palms and soles may predominate. Mucosal involvement in children is common.
Genital involvement is reported to occur in less than 50% of cases. Localized bullous pemphigoid of the genital skin is reported in children aged 7-12. Girls are affected more frequently than boys. When present, this condition can be misdiagnosed as child sexual abuse, and careful consideration must be taken in these cases.
The natural history of bullous pemphigoid in pediatric patients is not well characterized, but some have been reported to resolve within 1-2 years, while others have had a relapsing course.
Bullous pemphigoid is a chronic autoimmune subepidermal vesiculobullous disease that is most common in older adults. It is rarely seen in infants and children, in whom the precise incidence is unknown.
In the pediatric population, clinical presentation of bullous pemphigoid is variable, with ill-appearing patients who have severe, generalized blisters on one end of the spectrum and patients with localized, asymptomatic lesions on the other. As in adults, pruritic urticarial papules and plaques may precede the formation of bullae. Bullae can be widespread or localized on any body surface. In infants, palms and soles may predominate. Mucosal involvement in children is common.
Genital involvement is reported to occur in less than 50% of cases. Localized bullous pemphigoid of the genital skin is reported in children aged 7-12. Girls are affected more frequently than boys. When present, this condition can be misdiagnosed as child sexual abuse, and careful consideration must be taken in these cases.
The natural history of bullous pemphigoid in pediatric patients is not well characterized, but some have been reported to resolve within 1-2 years, while others have had a relapsing course.
Codes
ICD10CM:
L12.0 – Bullous pemphigoid
SNOMEDCT:
402439006 – Childhood bullous pemphigoid
L12.0 – Bullous pemphigoid
SNOMEDCT:
402439006 – Childhood bullous pemphigoid
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:03/01/2022
Last Updated:03/02/2022
Last Updated:03/02/2022