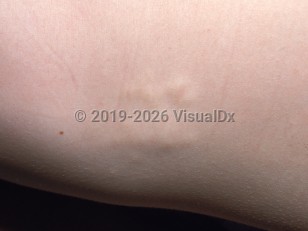
Buschke-Ollendorff syndrome in Adult
Alerts and Notices
Important News & Links
Synopsis

Buschke-Ollendorff syndrome (BOS) is a rare autosomal dominant disorder featuring connective tissue nevi and/or skeletal abnormalities. Incidence is thought to be 1:20 000. The clinical presentation is variable and may include any combination of collagen-rich connective tissue nevi (dermatofibrosis lenticularis disseminata), elastomas, osteopoikilosis, and melorheostosis.
BOS is caused by a loss-of-function mutation in LEMD3, which encodes a nuclear membrane protein, MAN1. Elastin production is higher than normal in both involved and uninvolved skin; lesional fibroblasts have been estimated to produce up to 8 times more tropoelastin (elastin precursor) than control fibroblasts. This condition is characterized by variable expressivity, evidenced when comparing individuals with mutations in LEMD3, even within the same family. It has been postulated that the presence of melorheostosis may represent acquisition of an additional somatic mutation in LEMD3 in the affected areas. Scoliosis has also been associated with LEMD3 mutations. Some patients have only skeletal manifestations derived from similar LEMD3 mutations; they are considered to have autosomal dominant osteopoikilosis.
Patients develop the characteristic connective tissue nevi in the first 2 decades of life, with osteopoikilosis developing before puberty. Bone findings are typically incidental, as the lesions are mostly asymptomatic. Limb length discrepancy has been reported. There are reports of joint pain and stiffness, usually with underlying osteopoikilosis or melorheostosis. Spinal stenosis may also be associated with osteopoikilosis.
There is usually no increased morbidity associated with this syndrome, but diagnosis may help prevent costly medical workup. One family had an association with late onset morphea. One patient with extensive cutaneous findings also had joint stiffness and hoarseness due to lingual elastosis and leukoplakia.
BOS is caused by a loss-of-function mutation in LEMD3, which encodes a nuclear membrane protein, MAN1. Elastin production is higher than normal in both involved and uninvolved skin; lesional fibroblasts have been estimated to produce up to 8 times more tropoelastin (elastin precursor) than control fibroblasts. This condition is characterized by variable expressivity, evidenced when comparing individuals with mutations in LEMD3, even within the same family. It has been postulated that the presence of melorheostosis may represent acquisition of an additional somatic mutation in LEMD3 in the affected areas. Scoliosis has also been associated with LEMD3 mutations. Some patients have only skeletal manifestations derived from similar LEMD3 mutations; they are considered to have autosomal dominant osteopoikilosis.
Patients develop the characteristic connective tissue nevi in the first 2 decades of life, with osteopoikilosis developing before puberty. Bone findings are typically incidental, as the lesions are mostly asymptomatic. Limb length discrepancy has been reported. There are reports of joint pain and stiffness, usually with underlying osteopoikilosis or melorheostosis. Spinal stenosis may also be associated with osteopoikilosis.
There is usually no increased morbidity associated with this syndrome, but diagnosis may help prevent costly medical workup. One family had an association with late onset morphea. One patient with extensive cutaneous findings also had joint stiffness and hoarseness due to lingual elastosis and leukoplakia.
Codes
ICD10CM:
Q78.8 – Other specified osteochondrodysplasias
SNOMEDCT:
60399005 – Dermatofibrosis lenticularis disseminata
Q78.8 – Other specified osteochondrodysplasias
SNOMEDCT:
60399005 – Dermatofibrosis lenticularis disseminata
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:09/09/2020
Last Updated:01/12/2022
Last Updated:01/12/2022
Buschke-Ollendorff syndrome in Adult