- Immunocompetent adults: common etiologies include Staphylococcus aureus (particularly if there is concurrent purulence) and Streptococcus pyogenes.
- Immunocompromised individuals: common pathogens such as S aureus and Streptococcus should be considered, but gram-negative pathogens should also be considered and covered.
- Diabetic foot infections and decubitus ulcers: consider a mixture of gram-positive cocci and gram-negative aerobes and anaerobes.
- Aquatic soft tissue injury: Vibrio spp, Aeromonas spp, Mycobacterium marinum, etc.
Risk factors for developing cellulitis include minor skin trauma, atopic dermatitis, contact dermatitis, body piercings, intravenous (IV) drug use, tinea pedis infection, animal bites, peripheral vascular disease, obesity, older age, immune suppression (chronic systemic steroid use, neutropenia, immunosuppressive medications, organ transplantation, HIV), and lymphatic damage (lymph node dissection, radiation therapy, vein harvest for coronary artery bypass surgery / saphenous venectomy, and damage that occurs following multiple prior episodes of cellulitis).
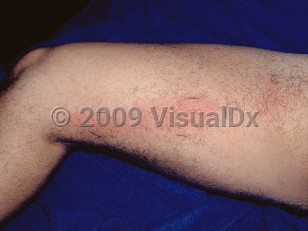
Fevers, chills, and malaise may precede the onset of cellulitis but may also be absent. Poorly defined borders, erythema, swelling, tenderness, and warmth characterize typical cellulitis lesions. In adults, the extremities, particularly the lower extremities, are the most common sites affected. In more severe cases, additional clinical features may include vesicle and bullae formation, pustules, and necrosis. Complications are not common but can include glomerulonephritis, lymphadenitis, and bacteremia.
A rising prevalence of MRSA has been identified as a pathogen of skin and soft tissue infections in otherwise healthy individuals lacking the aforementioned risk factors for cellulitis. MRSA should be considered for penetrating traumas, purulent infections, and in specific populations: athletes, children, prisoners, military service members, long-term care residents, and IV drug users. Other MRSA risk factors include recent admission to a health care facility, presence of an indwelling catheter, poor personal hygiene, and history of MRSA.
Recurrent Cellulitis: Major risk factors for recurrent cellulitis include chronic edema, dermatomycosis, and lymphatic or venous insufficiency. Prior episodes of cellulitis, immunodeficient states, obesity, previous local surgery / saphenectomy, as well as having cancer, can also increase the risk of recurrent cellulitis.
Note: It is exceedingly rare for cellulitis to occur bilaterally simultaneously, so if redness and involvement of the legs are bilateral in a patient suspected to have cellulitis, consider an alternative diagnosis such as stasis dermatitis or contact dermatitis (allergic, irritant).
Related topics: orbital cellulitis, preseptal cellulitis



 Patient Information for
Patient Information for