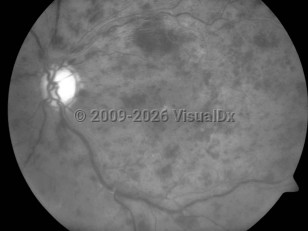
Central retinal vein occlusion - External and Internal Eye
Alerts and Notices
Important News & Links
Synopsis

The central retinal artery and vein share a common adventitial sheath as they exit the optic nerve head and pass through the lamina cribrosa. Often in CRVO, a rigid atherosclerotic artery impinges on the nearby vein, causing turbulence and predisposing to thrombus formation. With increased resistance of venous flow, the retina becomes ischemic and fluid leaks out of the vessels. Increased intraocular pressure could also cause turbulence of the central retinal vein and lead to thrombus formation and obstruction.
The occluded central vein can lead to intraretinal hemorrhage, exudation of fluid, varying levels of ischemia, and neovascular complications such as neovascular glaucoma. CRVO is commonly classified by severity into 2 forms: the nonischemic form of CRVO, which is milder and more common, and the ischemic form, which results in more severe retinal damage and vision loss. In ischemic CRVO, more than 90% of patients have vision of 20/400 or worse. One-third of patients with the nonischemic type progress to the ischemic type.
Iris neovascularization, which is associated with neovascular glaucoma, occurs in up to 60% of patients with the ischemic form, usually 3-5 months following the obstruction. The main risk factors for development of neovascular glaucoma after a CRVO are the extent of capillary nonperfusion, poor visual acuity, severe venous tortuosity, and retinal hemorrhage.
The presenting visual acuity at the time of diagnosis of CRVO is the best predictor of visual prognosis. In a patient with CRVO, there is a 10% risk of developing a CRVO in the fellow eye, especially when there is an underlying systemic abnormality.
Codes
H34.8191 – Central retinal vein occlusion, unspecified eye, with retinal neovascularization
SNOMEDCT:
68478007 – Central retinal vein occlusion
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:12/17/2012