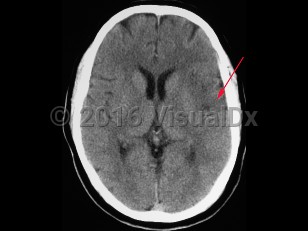
Strokes can be classified in the following way, with clinical presentation based on type.
Ischemic stroke:
- Thrombotic stroke – Secondary to thrombus formation that produces a stroke due to reduced distal blood flow or to an embolic fragment that breaks off and travels distally, causing occlusion (thromboembolic). Thrombotic strokes may occur in either large or small vessels. Clinical symptoms typically follow the affected vascular pattern. Cerebral venous sinus thrombosis is a rare cause of stroke.
- Embolic stroke – Embolic sources include cardiac (cardioembolic) due to arrhythmias and low flow states (atrial fibrillation, atrial flutter), or structural abnormalities (valvular or wall motion abnormalities), or arterial-to-arterial sources from a ruptured plaque (thromboembolic). Clinical symptoms are usually abrupt in onset and may have less localized effects due to the wide areas affected by embolic showering if more than 1 embolus is put into the circulation.
- Cerebral hypoperfusion – Secondary to systemic hypoperfusion due to cardiac arrhythmia, heart failure, pulmonary embolus, or sepsis. Patients often present with global cerebral dysfunction, and the so-called watershed areas between major cerebral artery perfusion areas are most often affected.
- Intracerebral hemorrhage – Bleeding directly into the brain parenchyma secondary to hypertension, trauma, bleeding disorders, aneurysm rupture, illicit drug use, or vascular malformations. Patients typically present with the gradual onset of symptoms over hours to days with headache, nausea, vomiting, and altered levels of consciousness. If the source of the hemorrhage is from the low-pressure side of the circulation, then the onset of symptoms is more likely to be gradual than if the source is from the high-pressure, arterial side, where symptoms can be quite abrupt in onset. Patients can also present with seizure.
- Subarachnoid hemorrhage – Bleeding directly into the cerebrospinal fluid (CSF) within the subarachnoid space that surrounds the brain due to either an arterial aneurysm at the base of the brain or bleeding from vascular malformation at the pial surface. Onset of symptoms is typically acute with a severe widespread headache, radiation of pain down the neck and back, and vomiting. Meningismus may be present.
Increased alcohol intake as well as illicit drugs, especially cocaine, methamphetamine, and heroin, increase stroke risk. Certain blood disorders such as sickle cell anemia and polycythemia are associated with stroke. Other risk factors include obstructive sleep apnea, chronic kidney disease, oral contraceptive use, and malignancy. Increased urinary sodium is associated with increased risk.
Risk factors for hemorrhagic stroke include hypertension, age, use of anticoagulants, arteriovenous malformations, and use of illicit drugs like cocaine.
This is a medical emergency and requires prompt evaluation!
Related topics: childhood stroke, drug-induced stroke, perinatal stroke