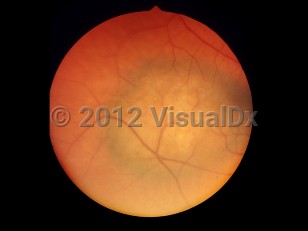
Choroidal melanoma - External and Internal Eye
Alerts and Notices
Important News & Links
Synopsis

Choroidal melanoma, a form of uveal melanoma, is the most common primary intraocular tumor of adults, with an incidence in the United States of 6 cases per million. It is 15 times less common than cutaneous melanoma and mainly affects individuals aged 60-70 years.
The most important risk factors include older age, light eye color, light skin, and chronic sun exposure. Other risk factors include ocular melanocytic conditions such as oculodermal melanocytosis (nevus of Ota) and melanosis oculi. Choroidal nevus, a common benign tumor found on the fundus, may rarely transform to melanoma. Choroidal melanoma is rarely hereditary; these cases account for less than 1% of tumors. A very small increase in risk of ocular melanoma has been described in those with BRCA2 gene mutations and other germline mutations.
Patients often present without any symptoms, and the choroidal melanoma is found incidentally on routine eye examination. Patients sometimes complain of blurred vision, floaters, photopsia, or visual field defects.
About 50% of patients will go on to have metastatic disease. The most common sites of metastasis include liver, lung, and bone. Brain and lymph node metastases can occur but are rare. Survival rates are generally poor, particularly if metastasis is found. The Collaborative Ocular Melanoma Study (COMS), a large multicenter randomized controlled trial, showed improved survival with younger age and smaller maximum basal tumor diameter. Five-year rates of death with histopathologically confirmed metastasis were 1%, 10%, and 33% for patients found to have, respectively, small (tumors 4-8 mm in largest basal diameter and 1-2.4 mm in thickness), medium (6-12 mm base diameter and 2.5-8 mm in thickness), and large (greater than 12 mm in largest basal diameter and 8 mm in thickness) ocular melanomas without metastasis at baseline. Chromosomal 3 monosomy also correlates strongly with metastatic disease and mortality.
The most important risk factors include older age, light eye color, light skin, and chronic sun exposure. Other risk factors include ocular melanocytic conditions such as oculodermal melanocytosis (nevus of Ota) and melanosis oculi. Choroidal nevus, a common benign tumor found on the fundus, may rarely transform to melanoma. Choroidal melanoma is rarely hereditary; these cases account for less than 1% of tumors. A very small increase in risk of ocular melanoma has been described in those with BRCA2 gene mutations and other germline mutations.
Patients often present without any symptoms, and the choroidal melanoma is found incidentally on routine eye examination. Patients sometimes complain of blurred vision, floaters, photopsia, or visual field defects.
About 50% of patients will go on to have metastatic disease. The most common sites of metastasis include liver, lung, and bone. Brain and lymph node metastases can occur but are rare. Survival rates are generally poor, particularly if metastasis is found. The Collaborative Ocular Melanoma Study (COMS), a large multicenter randomized controlled trial, showed improved survival with younger age and smaller maximum basal tumor diameter. Five-year rates of death with histopathologically confirmed metastasis were 1%, 10%, and 33% for patients found to have, respectively, small (tumors 4-8 mm in largest basal diameter and 1-2.4 mm in thickness), medium (6-12 mm base diameter and 2.5-8 mm in thickness), and large (greater than 12 mm in largest basal diameter and 8 mm in thickness) ocular melanomas without metastasis at baseline. Chromosomal 3 monosomy also correlates strongly with metastatic disease and mortality.
Codes
ICD10CM:
C69.30 – Malignant neoplasm of unspecified choroid
SNOMEDCT:
255021005 – Malignant melanoma of choroid
C69.30 – Malignant neoplasm of unspecified choroid
SNOMEDCT:
255021005 – Malignant melanoma of choroid
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:09/20/2022
Last Updated:04/10/2024
Last Updated:04/10/2024