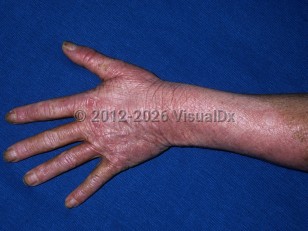
Chronic actinic dermatitis
Alerts and Notices
Important News & Links
Synopsis

Although the etiology is unclear, one proposed pathophysiologic mechanism is that CAD results from photoinduced modification of endogenous cutaneous antigen(s).
CAD is most commonly seen in men aged older than 50 years, with a long history of either occupational or recreational outdoor activities. The condition can be seen in women and also rarely in younger patients. Affected patients of all ages often have a history of atopic dermatitis and/or a history of allergic contact dermatitis and thus have a baseline tendency for delayed-type hypersensitivity reactions. CAD can occur in any skin type and anywhere in the world, although it is more commonly seen in patients with Fitzpatrick skin types V and VI and in temperate climates.
CAD may be a presenting sign of HIV infection, especially in younger CAD patients. If the diagnosis of CAD is considered, testing for HIV is recommended for patients with positive risk factors for HIV.
Codes
L57.1 – Actinic reticuloid
SNOMEDCT:
52636001 – Actinic reticuloid
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/07/2021