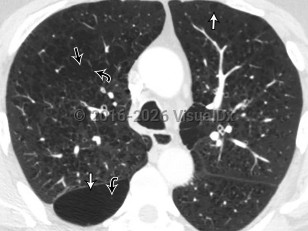
Chronic obstructive pulmonary disease
Alerts and Notices
Important News & Links
Synopsis

Emergent Care / Stabilization:
Acute exacerbations often require systemic steroids and standing nebulized bronchodilators. In serious cases, patients may require support with noninvasive positive pressure ventilation such as bilevel positive airway pressure (BiPAP) and in severe cases may require invasive ventilation and intensive care unit (ICU) admission.
Diagnosis Overview:
Chronic obstructive pulmonary disease (COPD) is a preventable and treatable condition with both pulmonary and extrapulmonary effects. Despite this, it is the third leading cause of death worldwide. COPD is characterized by chronic airflow obstruction that is not fully reversible. The disease is usually progressive and due to an abnormal inflammatory response in the lungs. Extrapulmonary manifestations include systemic inflammation, weight loss / nutritional deficiency, anemia, skeletal muscle dysfunction, and an increased risk for cardiovascular comorbidities.
Risk factors for the development of COPD include cigarette smoke exposure (primary or secondary) and occupational exposures (organic and inorganic dusts, chemical fumes, and smoke) as well as biomass fuel smoke exposure (from combustion of fuel developed from plant or animal materials, eg, wood, crops, animal waste, and some municipal solid waste) in the developed setting. Patients with alpha-1 antitrypsin deficiency, an inherited disorder, are at increased risk for developing COPD, including at a younger age.
COPD due to cigarette smoke exposure leads to more severe emphysema and more rapid decline in lung function compared with COPD from biomass exposure. The latter presents with distinctive airway wall thickening and sees lung function improve from the use of bronchodilators. The number of symptoms, exacerbations, and hospitalizations is higher in patients with asthma leading to COPD compared with patients with smoking-associated COPD, although, paradoxically, the asthma-associated mortality rate is lower.
Eosinophilic COPD represents a distinct subgroup of COPD patients with increased corticosteroid response. It has been labeled as a part of the asthma-COPD overlap syndrome, although these patients are often notable for having serum eosinophilia > 3%. Of note, unlike other patients with asthma-COPD overlap syndrome, eosinophilic COPD patients tend to be older and have fewer environmental allergies and fewer overall exacerbations. It is not clear that these subcategories of COPD should impact the approach to management, however.
Most patients with COPD present with cough and dyspnea, symptoms that often have developed insidiously by the time the patient finally presents to care. Chronic daily cough is predictive of frequent exacerbations. Per the Global Initiative for Chronic Obstructive Lung Disease (GOLD) guidelines, a post-bronchodilator forced expiratory volume in 1 second (FEV-1) / forced vital capacity (FVC) ratio of less than 70% defines COPD. The FEV-1 (% predicted) determines severity.
Hypertension is the most common concurrent disease in patients with COPD. Other common coexisting conditions include ischemic heart disease, atrial fibrillation, heart failure, osteoporosis, lung cancer, gastroesophageal reflux, anxiety, and depression, all of which may occur at younger ages in patients with COPD than in the general population.
Acute exacerbations often require systemic steroids and standing nebulized bronchodilators. In serious cases, patients may require support with noninvasive positive pressure ventilation such as bilevel positive airway pressure (BiPAP) and in severe cases may require invasive ventilation and intensive care unit (ICU) admission.
Diagnosis Overview:
Chronic obstructive pulmonary disease (COPD) is a preventable and treatable condition with both pulmonary and extrapulmonary effects. Despite this, it is the third leading cause of death worldwide. COPD is characterized by chronic airflow obstruction that is not fully reversible. The disease is usually progressive and due to an abnormal inflammatory response in the lungs. Extrapulmonary manifestations include systemic inflammation, weight loss / nutritional deficiency, anemia, skeletal muscle dysfunction, and an increased risk for cardiovascular comorbidities.
Risk factors for the development of COPD include cigarette smoke exposure (primary or secondary) and occupational exposures (organic and inorganic dusts, chemical fumes, and smoke) as well as biomass fuel smoke exposure (from combustion of fuel developed from plant or animal materials, eg, wood, crops, animal waste, and some municipal solid waste) in the developed setting. Patients with alpha-1 antitrypsin deficiency, an inherited disorder, are at increased risk for developing COPD, including at a younger age.
COPD due to cigarette smoke exposure leads to more severe emphysema and more rapid decline in lung function compared with COPD from biomass exposure. The latter presents with distinctive airway wall thickening and sees lung function improve from the use of bronchodilators. The number of symptoms, exacerbations, and hospitalizations is higher in patients with asthma leading to COPD compared with patients with smoking-associated COPD, although, paradoxically, the asthma-associated mortality rate is lower.
Eosinophilic COPD represents a distinct subgroup of COPD patients with increased corticosteroid response. It has been labeled as a part of the asthma-COPD overlap syndrome, although these patients are often notable for having serum eosinophilia > 3%. Of note, unlike other patients with asthma-COPD overlap syndrome, eosinophilic COPD patients tend to be older and have fewer environmental allergies and fewer overall exacerbations. It is not clear that these subcategories of COPD should impact the approach to management, however.
Most patients with COPD present with cough and dyspnea, symptoms that often have developed insidiously by the time the patient finally presents to care. Chronic daily cough is predictive of frequent exacerbations. Per the Global Initiative for Chronic Obstructive Lung Disease (GOLD) guidelines, a post-bronchodilator forced expiratory volume in 1 second (FEV-1) / forced vital capacity (FVC) ratio of less than 70% defines COPD. The FEV-1 (% predicted) determines severity.
Hypertension is the most common concurrent disease in patients with COPD. Other common coexisting conditions include ischemic heart disease, atrial fibrillation, heart failure, osteoporosis, lung cancer, gastroesophageal reflux, anxiety, and depression, all of which may occur at younger ages in patients with COPD than in the general population.
Codes
ICD10CM:
J44.9 – Chronic obstructive pulmonary disease, unspecified
SNOMEDCT:
13645005 – Chronic obstructive lung disease
J44.9 – Chronic obstructive pulmonary disease, unspecified
SNOMEDCT:
13645005 – Chronic obstructive lung disease
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:05/13/2025
Last Updated:05/18/2025
Last Updated:05/18/2025
Chronic obstructive pulmonary disease