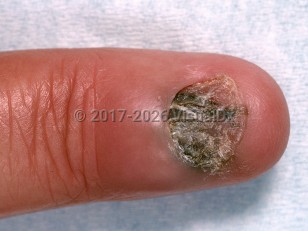
Chronic paronychia - Nail and Distal Digit
Alerts and Notices
Important News & Links
Synopsis

Chronic paronychia is defined as inflammation of a nail fold (the skin surrounding the fingernails) that lasts longer than 6 weeks. Symptoms may include redness, swelling, and sometimes pain. Fluctuance is absent. There may be disruption or absence of the cuticle, and protracted cases may manifest with changes in the nail plate itself, including grooves and ridges. Nail plate involvement signals damage to the nail matrix, which lies deep to and proximal to the proximal nail fold. Acute paronychia with marked tenderness, erythema, and even abscess formation may complicate chronic paronychia or precede it.
There is debate as to whether chronic paronychia is primarily an infectious or an inflammatory disease process; the current view is that chronic paronychia is a species of chronic irritant or allergic hand dermatitis. Evidence includes frequent association with occupational exposures in dishwashers, bartenders, laundry workers, nurses, swimmers, fishmongers, and cooks and a study demonstrating the superiority of treatment with potent topical steroids over systemic antifungals. Women are more frequently affected than men. It usually affects multiple fingernails.
Infectious pathogens also play a role in this condition. The chronic inflammatory process compromises the nail fold barrier to entry of microorganisms. Superinfection with bacteria may result in acute paronychia as a sequela. Fungal colonization and/or infection, especially with Candida albicans, is common. In one study, Candida was cultured in over 90% of patients with chronic paronychia.
Certain drugs can cause drug-induced paronychia (potentially either acute or chronic). These include retinoids (isotretinoin, acitretin), methotrexate, antiretroviral protease inhibitors (indinavir, lamivudine), and epidermal growth factor (EGF) receptor inhibitors (cetuximab, gefitinib, lapatinib). In some cases, drug-induced paronychia is associated with periungual lobular capillary hemangiomas (pyogenic granulomas).
Diabetes mellitus, immunosuppression, and inflammatory dermatoses are risk factors for developing chronic paronychia.
There is debate as to whether chronic paronychia is primarily an infectious or an inflammatory disease process; the current view is that chronic paronychia is a species of chronic irritant or allergic hand dermatitis. Evidence includes frequent association with occupational exposures in dishwashers, bartenders, laundry workers, nurses, swimmers, fishmongers, and cooks and a study demonstrating the superiority of treatment with potent topical steroids over systemic antifungals. Women are more frequently affected than men. It usually affects multiple fingernails.
Infectious pathogens also play a role in this condition. The chronic inflammatory process compromises the nail fold barrier to entry of microorganisms. Superinfection with bacteria may result in acute paronychia as a sequela. Fungal colonization and/or infection, especially with Candida albicans, is common. In one study, Candida was cultured in over 90% of patients with chronic paronychia.
Certain drugs can cause drug-induced paronychia (potentially either acute or chronic). These include retinoids (isotretinoin, acitretin), methotrexate, antiretroviral protease inhibitors (indinavir, lamivudine), and epidermal growth factor (EGF) receptor inhibitors (cetuximab, gefitinib, lapatinib). In some cases, drug-induced paronychia is associated with periungual lobular capillary hemangiomas (pyogenic granulomas).
Diabetes mellitus, immunosuppression, and inflammatory dermatoses are risk factors for developing chronic paronychia.
Codes
ICD10CM:
B37.2 – Candidiasis of skin and nail
SNOMEDCT:
200744008 – Chronic paronychia
B37.2 – Candidiasis of skin and nail
SNOMEDCT:
200744008 – Chronic paronychia
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:07/25/2017
Last Updated:02/14/2022
Last Updated:02/14/2022
 Patient Information for Chronic paronychia - Nail and Distal Digit
Patient Information for Chronic paronychia - Nail and Distal Digit
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Chronic paronychia - Nail and Distal Digit