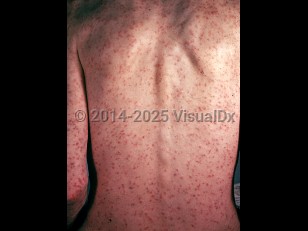
Colorado tick fever
Alerts and Notices
Important News & Links
Synopsis

Colorado tick fever (CTF) is one of the tickborne diseases that are collectively referred to as mountain fever or mountain tick fever because of their occurrence in the United States' Rocky Mountains. CTF is considered the less important cause of mountain fever (the other cause being Rocky Mountain spotted fever), with only about 200-400 cases occurring annually.
This tickborne illness is caused by a coltivirus from the Reoviridae family called the Colorado tick fever virus (CTFV). The Dermacentor andersoni tick (Rocky Mountain wood tick) is the primary vector. This acarian is usually found at elevations of 4 000-10 000 feet. The disease is endemic to the Rocky Mountains of the United States and Canada. The larva or nymph of the tick acquires the virus by feeding on viremic small mammals, such as voles, chipmunks, rabbits, marmots, and deer, and then it transmits it to humans through bites. Rarely, humans may also acquire CTF through blood transfusions. Transmission occurs seasonally with peak periods of risk between April and June, but it can also occur from March to September.
The incubation period is typically 2-6 days but may be as early as 1 day and as late as 20 days. The majority of CTF infections are self-limiting, but more severe disease presents with an abrupt onset of a triad of symptoms that include fever (40°C [104°F]), severe myalgia, arthralgia, and headaches. Chills, photophobia, and retro-orbital pain associated with conjunctival injection are some of the complaints reported by patients. About 25% of cases may also have abdominal pain, nausea, vomiting, and diarrhea. Pharyngitis occurs in about 20% of patients. Patients may exhibit lethargy, generalized weakness, and prostration with nuchal rigidity. Splenomegaly may be present.
Fever occurring in CTF is described as "saddleback fever" because of its biphasic pattern consisting of 2 spikes separated by an interval of 2-3 days. This is typically followed by a 2 to 3-day defervescence, then recurrence. Higher temperatures are usually reached during the second phase. During the febrile period, patients may experience flushing and tachycardia proportional to the temperature rise.
Neurologic symptoms, if present, usually commence within 7 days of the onset of illness and may range from clouded sensorium to somnolence or even coma.
Fewer than 15% of patients have dermatologic manifestations, which include a macular-petechial rash that occurs, especially during febrile episodes. Complications of CTF occur more commonly in children and when there is a delay in diagnosis. These include meningitis, encephalitis, hepatitis, gastrointestinal hemorrhage, pneumonitis, myocarditis, disseminated intravascular coagulopathy, epididymo-orchitis, and a rheumatic fever-like syndrome. The incidence of complications has been reported to be less than or equal to 7%. Barring the onset of complications, symptoms usually subside within 1 week. Convalescence is age dependent, with patients younger than 20 showing a complete recovery. In patients aged older than 30, 70% may continue to experience fatigue, lassitude, and asthenia for weeks to months.
This tickborne illness is caused by a coltivirus from the Reoviridae family called the Colorado tick fever virus (CTFV). The Dermacentor andersoni tick (Rocky Mountain wood tick) is the primary vector. This acarian is usually found at elevations of 4 000-10 000 feet. The disease is endemic to the Rocky Mountains of the United States and Canada. The larva or nymph of the tick acquires the virus by feeding on viremic small mammals, such as voles, chipmunks, rabbits, marmots, and deer, and then it transmits it to humans through bites. Rarely, humans may also acquire CTF through blood transfusions. Transmission occurs seasonally with peak periods of risk between April and June, but it can also occur from March to September.
The incubation period is typically 2-6 days but may be as early as 1 day and as late as 20 days. The majority of CTF infections are self-limiting, but more severe disease presents with an abrupt onset of a triad of symptoms that include fever (40°C [104°F]), severe myalgia, arthralgia, and headaches. Chills, photophobia, and retro-orbital pain associated with conjunctival injection are some of the complaints reported by patients. About 25% of cases may also have abdominal pain, nausea, vomiting, and diarrhea. Pharyngitis occurs in about 20% of patients. Patients may exhibit lethargy, generalized weakness, and prostration with nuchal rigidity. Splenomegaly may be present.
Fever occurring in CTF is described as "saddleback fever" because of its biphasic pattern consisting of 2 spikes separated by an interval of 2-3 days. This is typically followed by a 2 to 3-day defervescence, then recurrence. Higher temperatures are usually reached during the second phase. During the febrile period, patients may experience flushing and tachycardia proportional to the temperature rise.
Neurologic symptoms, if present, usually commence within 7 days of the onset of illness and may range from clouded sensorium to somnolence or even coma.
Fewer than 15% of patients have dermatologic manifestations, which include a macular-petechial rash that occurs, especially during febrile episodes. Complications of CTF occur more commonly in children and when there is a delay in diagnosis. These include meningitis, encephalitis, hepatitis, gastrointestinal hemorrhage, pneumonitis, myocarditis, disseminated intravascular coagulopathy, epididymo-orchitis, and a rheumatic fever-like syndrome. The incidence of complications has been reported to be less than or equal to 7%. Barring the onset of complications, symptoms usually subside within 1 week. Convalescence is age dependent, with patients younger than 20 showing a complete recovery. In patients aged older than 30, 70% may continue to experience fatigue, lassitude, and asthenia for weeks to months.
Codes
ICD10CM:
A93.2 – Colorado tick fever
SNOMEDCT:
6452009 – Colorado tick fever
A93.2 – Colorado tick fever
SNOMEDCT:
6452009 – Colorado tick fever
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:08/19/2018
Colorado tick fever