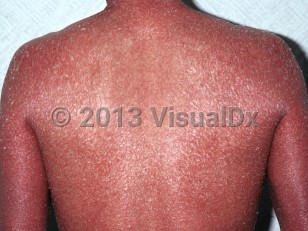
Several disorders, mostly with autosomal recessive inheritance and very rarely autosomal dominant inheritance, are included under this diagnosis. Some cases of harlequin ichthyosis may evolve into nonbullous CIE. These disorders are distinct from the lamellar ichthyosis form of nonbullous CIE, although at times this distinction is difficult.
Individuals may frequently have chronic secondary infection with dermatophytes, and rarely adults with this disorder have developed cutaneous squamous cell carcinomas.
Genes that are mutated and cause this condition include:
- ALOXE3 and ALOX12B – Genes involved with production of epidermal lipids.
- NIPAL4
- ABCA12 – Controls a liver transport protein and may cause severe forms of this disorder.
- Ichthyic mutations of a transmembrane protein.
- Some mutations of transglutaminase I may cause this form of nonbullous CIE.
- Patients with loss-of-function mutations in sphingosine-1-phosphate lyase may have nephrosis with ichthyosis and adrenal insufficiency.