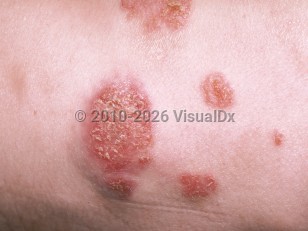
Cryptococcosis in Adult
See also in: Cellulitis DDxAlerts and Notices
Important News & Links
Synopsis

Primary inoculation cutaneous cryptococcosis may occur in normal and immunocompromised hosts, but infection is usually acquired by the respiratory route, with the lungs as the primary focus of the infection. In the presence of a normal immune system, the infection is usually contained and remains latent in the lung and/or hilar nodes. If there is subsequent immunosuppression, organisms may proliferate and cause symptomatic, active infection. In this situation, secondary hematogenous dissemination to the central nervous system (CNS), kidneys, larynx, and other organs, including the skin, occurs.
Pulmonary cryptococcosis may be heralded by chest pain and cough. In patients with HIV, it is usually more severe, especially with low CD4 counts. Headache, nausea, confusion, blurred vision, and abnormal gait may be presenting symptoms. Papilledema, cranial nerve palsies, mild fever, and mild meningismus may be present in some patients.
Cutaneous findings occur in 15%-20% of disseminated cases. The presentation is variable. Cellulitis, abscesses, papules, plaques, ulcers, sinus tracts, or purpura may all be seen. In patients with HIV, molluscum-like umbilicated papules are described.
Other possible sites of infection include the skeletal system, eyes, lymph nodes, liver, and genitourinary tract.
However, the presence of cryptococcal infection does not imply abnormal immune status; perhaps a quarter of patients have no predisposing condition. The disease has a 2:1 male predilection (even prior to AIDS).
Untreated disseminated disease is fatal. Mortality in patients with AIDS is 10%-25%.
Pediatric Patient Considerations:
Cryptococcus has been described in children without any immunodeficiency or antecedent conditions, although it most commonly occurs in children with immunodeficiencies such as HIV, status-post organ transplant, severe combined immunodeficiency syndrome, or hyperimmunoglobulin M syndrome.
Codes
B45.9 – Cryptococcosis, unspecified
SNOMEDCT:
42386007 – Cryptococcosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/10/2025