Risk factors for TB include poverty, being undomiciled, unemployment, crowding, and HIV infection. Approximately 8% of infections are seen in individuals infected with HIV; the risk of active TB in HIV-infected patients is 3%-8% per year with a lifetime risk of over 50%. Children are most susceptible to active TB with exposure, with 60%-80% developing active TB after exposure.
Cutaneous tuberculosis (CTB) is exceedingly rare, accounting for 1.5% -3% of extrapulmonary TB cases (8%-24% of TB infection is extrapulmonary). Approximately 1 out of 3 patients with CTB has systemic involvement with TB. CTB is more common in children, pregnant individuals, and HIV-infected persons.
CTB can be subclassified into 4 categories depending on route of infection: exogenous, endogenous, tuberculid, and vaccine-related.
Exogenous sources: Primary inoculation TB occurs at sites of trauma, abrasions, or wounds, or at mucous membranes.
- In patients with no immunity against TB, a scab or chancre forms at the wound site and can be associated with regional lymphadenopathy after several weeks. Lymph nodes can eventually suppurate, abscesses can form, and fever and pain can develop.
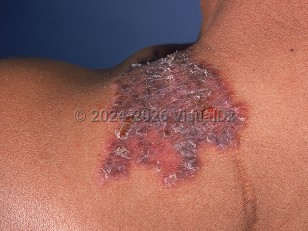
- In previously sensitized individuals, primary inoculation can lead to tuberculosis verrucosa cutis (warty tuberculosis) and is not usually associated with systemic symptoms.
- Scrofuloderma results from involvement of skin overlying a contiguous TB focus, usually a lymph node, bone, joint, or lacrimal gland. It is the most common form of CTB in children.
- Orificial TB is a rare mucosal autoinoculation TB from pulmonary, genitourinary, or intestinal disease shedding organisms that seed the adjacent orifices.
- Lupus vulgaris results from hematogenous spread and is a progressive form of CTB seen in individuals with prior sensitivity and low immunity.
- Tuberculous gumma (metastatic tuberculous abscess) is a rare form of hematogenous TB.
- Acute miliary TB is a rare but life-threatening form of hematogenous TB seen in patients with low immunity.
- Micropapular (lichen scrofulosorum)
- Papular (papulonecrotic tuberculid)
- Nodular (erythema induratum) – Characterized by tender erythematous nodules in the posterior legs. Lesions are typically asymptomatic but may be painful. Localized adenopathy may occur.
All forms of CTB, including tuberculids, require systemic treatment. Without treatment, lesions can persist for months to years. The prognosis of miliary TB is often poor.
Cutaneous manifestations of TB can also be broadly categorized into multibacillary versus paucibacillary forms (based on bacillary load).
Paucibacillary forms have a sparse number of bacteria:
- Lupus vulgaris
- TB verrucous cutis
- Tuberculids
- Scrofuloderma
- Orificial TB
- Acute miliary TB
- TB gumma
- Tuberculosis chancre