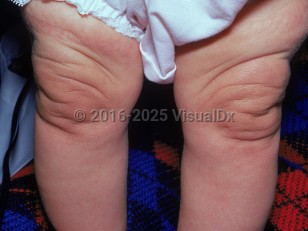
The AR forms are typically evident at birth and may be accompanied by early-onset emphysema:
- AR form, type 1 (1A-fibulin 5, 1B-fibulin 4, 1C-latent transforming growth factor [TGF] beta binding protein-4 gene mutations) – Characteristic skin findings beginning at birth. Systemic involvement is more severe, resulting in high mortality in early childhood.
- AR form, type 2 – Type 2A (wrinkled skin syndrome) is associated with defective N- and O-glycosylation. There is a strong female predominance. It is associated with severe neurologic manifestations including pachygyria, microcephaly, seizures, and Dandy-Walker malformation. Type 2B presents with wrinkled, inelastic skin, notably on the dorsal acral surfaces and abdomen, along with musculoskeletal and neurologic abnormalities. Patients display facial dysmorphism, with triangular facies and progeroid appearance.
- AR, type 3 (De Barsy syndrome / progeroid syndrome of De Barsy / cutis laxa-corneal clouding-intellectual disability syndrome) – Associated with bilateral corneal opacification, progeroid appearance, decreased subcutaneous fat, and athetoid movements beginning early in life.
The AD form, the mildest form with the fewest internal manifestations, is more likely to develop in later life, and patients have a normal lifespan.
Inherited syndromes with cutis laxa include:
- Macrocephaly, alopecia, cutis laxa, and scoliosis (MACS) syndrome – Notable for macrocephaly, facial dysmorphism, gingival hypertrophy, dental abnormalities, sparse hair, high-pitched voice, and musculoskeletal abnormalities. Ocular, neurologic, and respiratory symptoms are absent.
- Arterial tortuosity syndrome – AR disorder due to SLC2A10 mutation. There is variable skin laxity, cleft palate, hypertelorism, and bifid uvula. Arterial anomalies result in early death.
- Medication-induced cutis laxa causes acquired type 1 cutis laxa, sometimes with generalized elastolysis. Reported onset is within weeks to months of starting the medication. It has been associated with penicillin, isoniazid, and selective serotonin reuptake inhibitors (SSRIs). Neonatal cutis laxa can occur in newborns of birthing parents treated with penicillamine (or, less frequently, penicillin or isoniazid).
- Cutis laxa may be associated with urticaria or angioedema, malignancies (eg, multiple myeloma, lymphoma), congenital hemolytic anemia, arthropod bite reactions, extensive inflammatory skin disease (eg, atopic dermatitis, erythema multiforme, dermatitis herpetiformis, sarcoidosis, acute febrile neutrophilic dermatosis, interstitial granulomatous dermatitis), infections (eg, Toxocara canis, Borrelia burgdorferi, Treponema pallidum, Onchocerca volvulus), connective tissue diseases (eg, rheumatoid arthritis, systemic lupus erythematosus, lupus panniculitis), celiac disease, nephritic syndrome, alpha-1-antitrypsin deficiency, mastocytosis, and amyloidosis.
- Marshall syndrome – Also known as acquired cutis laxa type 2, this form of acquired cutis laxa is seen primarily in infants and young children following the onset of an inflammatory neutrophilic dermatosis.