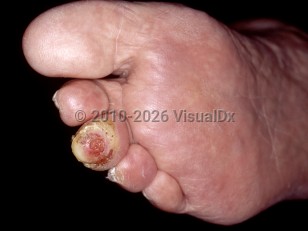
Diabetic neuropathy
Alerts and Notices
Important News & Links
Synopsis

Diabetic neuropathy is a chronic, pathological complication associated with diabetes mellitus, where nerve damage is incurred due to microvascular injury involving small blood vessels that supply nerves, resulting in peripheral sensory and motor and/or autonomic nerve dysfunction. Although commonly affecting distal and smaller nerves, infarction of proximal large nerves can also occur.
There may be a distal, often symmetric, polyneuropathy, or there may be focal or multifocal neuropathies. Symptoms typically include numbness, tingling, and/or burning pain in the extremities. Autonomic nerve dysfunction may occur and cause constipation, erectile dysfunction, dizziness, and urinary incontinence. If motor nerves are affected, patients may develop weakness. Symptoms usually progress. Diagnosis can be suspected in diabetic patients with classic symptoms, particularly those with poor glucose control.
Diabetic neuropathy usually develops after years of the disease and progresses slowly (years). Rapid progression is unusual.
Related topic: Charcot neuroarthropathy of the foot and ankle
There may be a distal, often symmetric, polyneuropathy, or there may be focal or multifocal neuropathies. Symptoms typically include numbness, tingling, and/or burning pain in the extremities. Autonomic nerve dysfunction may occur and cause constipation, erectile dysfunction, dizziness, and urinary incontinence. If motor nerves are affected, patients may develop weakness. Symptoms usually progress. Diagnosis can be suspected in diabetic patients with classic symptoms, particularly those with poor glucose control.
Diabetic neuropathy usually develops after years of the disease and progresses slowly (years). Rapid progression is unusual.
Related topic: Charcot neuroarthropathy of the foot and ankle
Codes
ICD10CM:
E13.40 – Other specified diabetes mellitus with diabetic neuropathy, unspecified
SNOMEDCT:
230572002 – Diabetic neuropathy
E13.40 – Other specified diabetes mellitus with diabetic neuropathy, unspecified
SNOMEDCT:
230572002 – Diabetic neuropathy
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:12/05/2016
Last Updated:11/07/2023
Last Updated:11/07/2023
Diabetic neuropathy