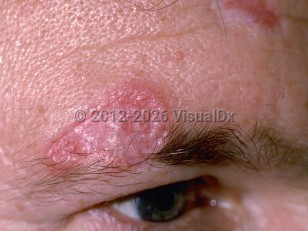
Discoid lupus erythematosus - Hair and Scalp
See also in: Overview,External and Internal EyeAlerts and Notices
Important News & Links
Synopsis

Discoid rash is one of 11 clinical criteria for the Systemic Lupus International Collaborating Centers (SLICC) classification of SLE and is a contributor to the musculoskeletal clinical domain within the European League Against Rheumatism / American College of Rheumatology (EULAR / ACR) classification criteria for SLE.
DLE may be localized or generalized. Localized DLE is limited to the face, scalp, ears, and neck, while in generalized DLE, there may be lesions both above and below the neck. It is rare for DLE to be isolated below the neck. There is a 20% likelihood of SLE with generalized DLE and 5% with localized DLE. Conversely, approximately 15%-30% of patients with SLE will manifest discoid lesions. Other risk factors for SLE include mucocutaneus involvement, arthralgias / arthritis, nail changes, anemia, leukopenia, an elevated ESR, and a positive antinuclear antibodies (ANA) test.
Squamous cell carcinoma may rarely develop in chronic DLE scars, especially in sun-exposed areas.
The presence of erythema multiforme-like lesions in a patient with lupus, along with a speckled pattern of ANA, positive anti-Ro/SSA or anti-La/SSB, and positive rheumatoid factor (RF) is known as Rowell syndrome. This syndrome has been described in patients with DLE, subacute cutaneous lupus erythematosus (SCLE), and SLE. Its existence as a distinct entity has been debated in the literature; some authors believe the association is coincidental. Prednisone with or without hydroxychloroquine, dapsone, or immunosuppressive drugs such as cyclosporine have been cited as therapy.
Related topics: drug-induced lupus erythematosus, lupus panniculitis, tumid lupus erythematosus
Codes
L93.0 – Discoid lupus erythematosus
SNOMEDCT:
200938002 – Discoid lupus erythematosus
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:04/10/2024
 Patient Information for Discoid lupus erythematosus - Hair and Scalp
Patient Information for Discoid lupus erythematosus - Hair and Scalp- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient