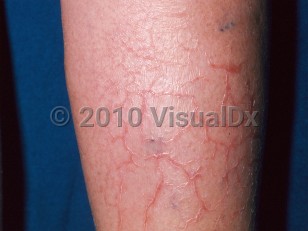
Eczema craquelé
Alerts and Notices
Important News & Links
Synopsis

Xerosis is the predisposing factor to the development of eczema craquelé. It refers to a condition of rough, dry skin texture with fine scale and occasionally fine fissuring. It is often pruritic. The pathogenesis involves a decrease in the amount of lipids in the stratum corneum and a deficiency in the water-binding capacity of this layer. The most common cause of xerosis is aging; however, it can be associated with a number of environmental factors and/or disease states, such as low humidity, frequent bathing, harsh soaps, congenital and acquired ichthyoses, atopic dermatitis, hypothyroidism, Down syndrome, renal failure, malnutrition and malabsorptive states, human immunodeficiency virus (HIV) infection, lymphoma, liver disease, Sjögren syndrome, carcinomatosis, and certain drugs. Asteatotic dermatitis is a rare presentation of zinc deficiency.
Eczema craquelé begins as dry skin that progresses to superficially fissured, inflamed, and sometimes crusted dermatitis. A generalized dermatitis can develop. The condition is seen mostly in elderly individuals. This may be due to decreased sebaceous / sweat gland activity and keratin synthesis in elderly persons, as well as a host of other factors such as malnutrition, drugs, and underlying illnesses. The condition is exacerbated by low humidity and frequent bathing without moisturizing. Pruritus is frequent, and painful lesions can occur if the fissures are deep.
Codes
L85.3 – Xerosis cutis
SNOMEDCT:
201077008 – Asteatotic eczema
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
 Patient Information for Eczema craquelé
Patient Information for Eczema craquelé - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient