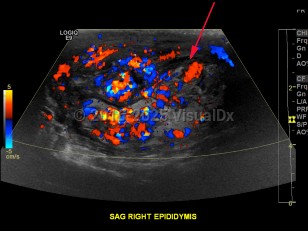
Epididymo-orchitis
Alerts and Notices
Important News & Links
Synopsis

Isolated orchitis can be caused by a variety of viral pathogens, including mumps (which is associated with orchitis with or without parotitis). Testicular atrophy may occur following an episode of viral orchitis. Most cases of isolated orchitis occur in postpubertal males and are unilateral. Less commonly, orchitis may occur in children and adolescents after viral or bacterial infection. Symptoms last from days to weeks. Rarely, epididymo-orchitis may be seen as complication of immunoglobulin A vasculitis.
Isolated epididymitis may be caused by trauma, but it is much more commonly caused by sexually transmitted pathogens (in military populations, in patients with a new sexual partner, or in patients with high-risk sexual behavior) or by enteric bacterial pathogens (older men and patients with recent manipulation of the genital tract, abnormalities of the genitourinary tract, or a history of bacterial prostatitis are at increased risk). In prepubertal boys, bacterial epididymitis is associated with genitourinary anomalies. The inflammation of the epididymis will typically progress to involve the testicles (epididymo-orchitis).
Symptoms of epididymo-orchitis usually develop over 1-2 days, although some patients will complain of a more gradual onset of symptoms. The primary complaint is swelling of the scrotum associated with pain. Urethral discharge is common. Fever may or may not be present. On palpation, swelling in the posterior scrotum localized over the involved epididymis can be appreciated. There may be a hydrocele. There may be erythema overlying the area of swelling. Pain should improve within 72 hours after treatment, although inflammation may persist for a few weeks.
If epididymo-orchitis is related to a sexually transmitted infection, the most common pathogens are Chlamydia trachomatis and Neisseria gonorrhoeae. In this case, antibiotic treatment should be directed against both pathogens. Testing for syphilis and HIV should be performed. Sexual partner identification and treatment is important from a public health perspective.
If the epididymo-orchitis is caused by an enteric bacterial pathogen (including Pseudomonas aeruginosa), a urine culture should be obtained and used to guide antimicrobial therapy.
If symptoms do not improve after initiating therapy, further diagnostic evaluation is warranted as patients may have epididymitis due to an unusual pathogen (eg, Mycobacterium tuberculosis or a fungal pathogen) or may have developed a complication of epididymitis such as an abscess or infarction.
Codes
N45.3 – Epididymo-orchitis
SNOMEDCT:
197983000 – Orchitis and epididymitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required