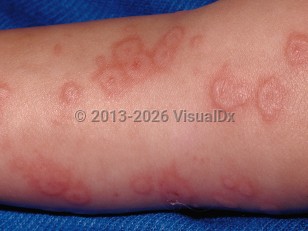
Erythema multiforme in Infant/Neonate
See also in: Anogenital,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

In older children and adults, herpes simplex virus (HSV) is a common etiology; however, HSV has not been reported as a significant etiology in infants. EM in neonates and infants is exceedingly rare. Reported triggers for infantile EM have included drugs (particularly penicillin), hepatitis, hepatitis B vaccination, Candida, and cow's milk.
Codes
L51.9 – Erythema multiforme, unspecified
SNOMEDCT:
36715001 – Erythema multiforme
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:12/20/2022
 Patient Information for Erythema multiforme in Infant/Neonate
Patient Information for Erythema multiforme in Infant/Neonate- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient