Recurrent EM occurs in a subset of patients and has been variably defined as more than 1, more than 2, or more than 6 flares per year.
Persistent EM is uncommon and refers to chronic, continuous presence of EM or outbreaks separated by 15 days or less.
In adults, the primary trigger for EM is herpes simplex virus (HSV), which is estimated to incite about 90% of cases. EM has been reported with other infections including histoplasmosis, Epstein-Barr virus, and, most recently, COVID-19. Medication can also be a trigger. In children, important additional triggers to consider include drugs (particularly penicillin), group A Streptococcus, and Epstein-Barr virus, among other viruses and bacteria. Idiopathic cases have also been seen.
Typically, all cutaneous lesions appear within 24-72 hours and persist for 1-4 weeks before fading. The eruption recurs on repeated exposure to the inciting agent.
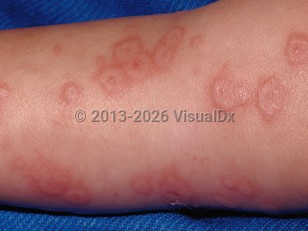
EM demonstrates classical target lesions, raised atypical target lesions, or both concomitantly on the skin.
The following points should be kept in mind when a diagnosis of EM is being considered:
- Herpes labialis may typically precede development of EM but may sometimes develop concomitantly or manifest after the onset of EM (In almost half of all cases, herpes labialis precedes EM.)
- Classical target lesions are well-defined circular lesions that are less than 3 cm in diameter and have 3 distinct color zones and a central zone that has a bulla or crust.
- Atypical target lesions are palpable, poorly defined, circular lesions that have 2 distinct color zones. Raised atypical targets are a subtype of atypical targets that have a vesicle or bulla centrally.
- EM is not considered within the same disease spectrum as Stevens-Johnson syndrome (SJS) / toxic epidermal necrolysis (TEN) and confers no risk of progressing to TEN.
- EM major refers to the presence of significant mucosal involvement in a case of EM, whereas in EM minor, mucosal involvement is absent or minimal.
- In EM major, painful intraoral and lip erosions eventuate from vesicles or bullae. Secondary crusting, including hemorrhagic crusting, then develops.



 Patient Information for
Patient Information for