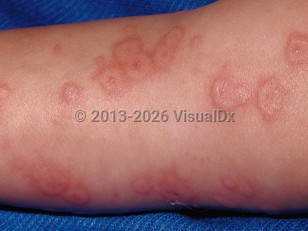
Erythema multiforme - Anogenital in
See also in: Overview,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Recurrent EM occurs in a subset of patients and has been variably defined as more than 1, more than 2, or more than 6 flares per year.
Persistent EM is uncommon and refers to chronic, continuous presence of EM or outbreaks separated by 15 days or less.
In adults, the primary trigger for EM is herpes simplex virus (HSV), which is estimated to incite about 90% of cases. EM has been reported with other infections including histoplasmosis, Epstein-Barr virus, and, most recently, COVID-19. Idiopathic cases have also been seen.
Typically, all cutaneous lesions appear within 24-72 hours and persist for 1-4 weeks before fading. The eruption recurs on repeated exposure to the inciting agent.
Codes
L51.9 – Erythema multiforme, unspecified
SNOMEDCT:
36715001 – Erythema multiforme
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:02/10/2023
 Patient Information for Erythema multiforme - Anogenital in
Patient Information for Erythema multiforme - Anogenital in - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient