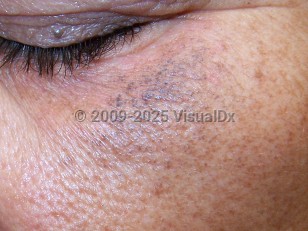
Exogenous ochronosis
Alerts and Notices
Important News & Links
Synopsis

The pigmentation usually presents as dark brown, black, or blue-black macules, particularly over the zygoma and orbital ridges, but any other facial surface or skin coming into chronic contact with causative agents may be affected. It may be preceded by erythema, and, in advanced cases, papules and nodules may ensue.
Exogenous ochronosis from topical hydroquinone has been reported most frequently in individuals with darker skin, but individuals with lighter skin may be affected as well. This difference may represent the differential use of hydroquinone in different populations. Onset has been reported as soon as 3 months of use. While the condition is usually associated with the prolonged use of skin lightening creams containing higher concentrations of hydroquinone, it has also been reported with the use of lower concentrations for shorter periods. In a 2022 systematic review, the majority of cases occurred in individuals who had used hydroquinone for more than a year, but ochronosis developed before a year as well. The high incidence in South Africa has been postulated to occur secondary to the use of unregulated products with higher hydroquinone concentrations and resorcinol and mercury additives.
The pathogenic mechanism is unclear, but the leading hypothesis suggests that hydroquinone and other known causative agents cause local inhibition of homogentisic acid (HGA) oxidase, an enzyme in the tyrosine metabolic pathway required to break down HGA, thereby leading to an accumulation of HGA in the skin. HGA then polymerizes and forms ochronotic pigments in the dermis.
Related topic: Alkaptonuria
Codes
L81.9 – Disorder of pigmentation, unspecified
SNOMEDCT:
410041002 – Exogenous ochronosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/30/2022