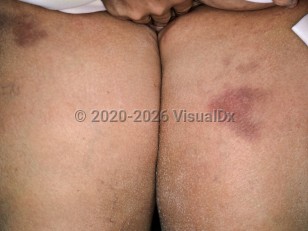
Mechanical causes – local pressure or repetitive blunt trauma
Physical causes – skin exposure to cold (eg, Popsicle or ice cube), heat, or electricity (eg, site of electrode, electrostimulation, or electroacupuncture needles)
Chemical causes – syringe or needle injection of disparate materials such as:
- Organic materials including acids, alkalis, milk, or microbiologically contaminated substances such as saliva, urine, or feces
- Cosmetic materials including bovine collagen, polymethyl methacrylate microspheres, and polydimethylsiloxane, and, less commonly, paraffin (mineral oil) and vegetable oils (cottonseed, sesame, or camphor oil)
- Therapeutic agents including vitamin K, povidone, meperidine, pentazocine, gold salts, vaccines (eg, tetanus antitoxoid), glatiramer acetate (treatment for multiple sclerosis), and cytotoxic chemotherapies (eg, anthracyclines, vinca alkaloids, or taxanes)
The atypical distribution of the lesions will often suggest an exogenous origin. However, the wide range of possible causes and lack of reliable patient history make the diagnosis of FP difficult, sometimes requiring multiple admissions before the cause of the lesions is discovered.
The inflammation is self-limited with minimal systemic symptoms unless there is concurrent infection. In these cases, the patient may develop abscesses and lymphangitic spread if not treated. In cases of deliberate self-injury, the subcutaneous inflammation may appear resistant to treatment or chronically recurring. However, when the affected areas are covered with bandages or protective casts, there is pronounced and rapid improvement.
Related topics: panniculitis, cold panniculitis, factitial dermatitis, factitial ulcer