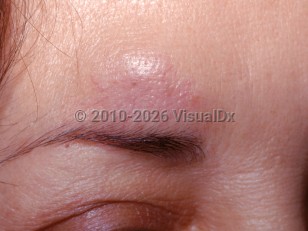
Foreign body granuloma can occur at any age and initially begins with acute inflammation at the site of entry of the foreign material. This is often followed by apparent resolution of the lesion. However, after a period of weeks, months, or even years, a chronic inflammatory reaction can ensue, presenting as a red or red-brown, inflamed, indurated papule, plaque, or nodule. Additional clinical findings may include cellulitis, abscess, edema, ulceration, and erythema.
The formation of a foreign body granuloma begins with neutrophils attracted to the site of entry. When the neutrophils are unable to engulf the foreign material, macrophages are attracted to the site. Macrophages become active and secrete cytokines once they have phagocytosed the foreign material. The secreted cytokines attract more macrophages and peripheral monocytes to the site of entry, and this process forms a chronic granuloma. Macrophages may fuse together to form multinucleated giant cells.
There are numerous causes of foreign body granuloma:
- Tattoo inks
- Paraffin
- Silicone (polydimethyl siloxane) liquid or gel
- Silica
- Talc
- Zirconium
- Beryllium
- Aluminum
- Zinc
- Other synthetic fillers, eg, poly-L-lactic acid, polymethylmethacrylate
- Hair keratin
- Pseudofolliculitis barbae
- Acne keloidalis nuchae
- 75% of sacrococcygeal pilonidal cysts
- Nail keratin
- Hair
- Bovine collagen
- Hyaluronic acid
- Starch
- Cactus spines
- Jellyfish and corals
- Sea urchin spines
- Silk sutures
- Corticosteroids
- Nylon or polypropylene sutures (used less frequently)
Accidental
- Wood splinters
- Cactus spines
- Blast injury
- Motor vehicle accident
- Talc or starch powders from surgical gloves
- Surgical sutures
- Laparoscopic gallbladder removal
- Gelfoam
- Aluminum chloride
- Ferric subsulfate (Monsel's solution)
- Hyaluronic acid fillers
- Bovine collagen fillers
- Silicone
- Paraffin for tissue augmentation
- Red pigment: cinnabar / mercuric sulfide (most common cause of granulomatous tattoo reaction)
- Blue pigment: cobalt
- Green pigment: chromium
- Yellow pigment: cadmium
- Purple pigment: manganese
- Black pigment: carbon (India ink)
- Brown pigment: ferric oxide
- White pigment: titanium or zinc oxide
- Zirconium oxide in deodorants and antipruritus preparations
- Intravenous drug users
- "Barber's interdigital pilonidal sinus" refers to the reaction surrounding an entrapped cut or shaved hair, often seen in an interdigital space of a barber's hand. These cases represent foreign body granulomas rather than true cysts.



 Patient Information for
Patient Information for