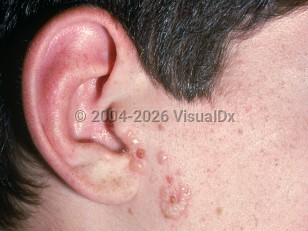
Gladiatorum herpes simplex virus in Adult
Alerts and Notices
Important News & Links
Synopsis

Herpes simplex virus (HSV) gladiatorum (HSVG), or herpes gladiatorum, is an HSV infection arising from nonsexual physical contact such as wrestling or other sporting activities. The causative agents for HSVG are the same viruses that cause classic herpes simplex: HSV-1 and HSV-2.
The exact incidence of herpes gladiatorum is not known, but usually it afflicts young and active individuals engaged in contact sports. The disease typically presents with an incubation period of about 3-5 days, followed by the eruption of painful grouped vesicles on an erythematous base. HSVG usually presents on the torso, legs, shoulders, neck, or forearms. In one large outbreak occurring at a high school wrestling training camp, HSVG was identified in 60 of 175 wrestlers, and most lesions were present on the head (73%), the extremities (42%), and the trunk (28%). Autoinoculation may result in infection at multiple sites on the body.
Depending on the intensity of the host response, a primary herpes infection, including HSVG, may be accompanied by systemic manifestations including fever, sore throat, headache, and lymphadenopathy.
Like all other HSV infections, the condition resolves with dormancy in the dorsal ganglia. During future periods of reduced immune function, repeat eruptions will occur in the same anatomic area as the primary infection. Scarring may also result from the eruption, and lesions close to the eyes may lead to herpes keratitis, an ophthalmologic emergency.
The exact incidence of herpes gladiatorum is not known, but usually it afflicts young and active individuals engaged in contact sports. The disease typically presents with an incubation period of about 3-5 days, followed by the eruption of painful grouped vesicles on an erythematous base. HSVG usually presents on the torso, legs, shoulders, neck, or forearms. In one large outbreak occurring at a high school wrestling training camp, HSVG was identified in 60 of 175 wrestlers, and most lesions were present on the head (73%), the extremities (42%), and the trunk (28%). Autoinoculation may result in infection at multiple sites on the body.
Depending on the intensity of the host response, a primary herpes infection, including HSVG, may be accompanied by systemic manifestations including fever, sore throat, headache, and lymphadenopathy.
Like all other HSV infections, the condition resolves with dormancy in the dorsal ganglia. During future periods of reduced immune function, repeat eruptions will occur in the same anatomic area as the primary infection. Scarring may also result from the eruption, and lesions close to the eyes may lead to herpes keratitis, an ophthalmologic emergency.
Codes
ICD10CM:
B00.1 – Herpesviral vesicular dermatitis
SNOMEDCT:
240475000 – Cutaneous herpes simplex infection
B00.1 – Herpesviral vesicular dermatitis
SNOMEDCT:
240475000 – Cutaneous herpes simplex infection
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:01/30/2017
Last Updated:01/26/2017
Last Updated:01/26/2017
 Patient Information for Gladiatorum herpes simplex virus in Adult
Patient Information for Gladiatorum herpes simplex virus in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Gladiatorum herpes simplex virus in Adult