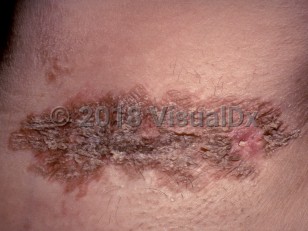
Granular parakeratosis in Adult
Alerts and Notices
Important News & Links
Synopsis

GP can occur in individuals of all ages and sexes. However, it is more common in women aged between 40 and 60 years, with a female-to-male ratio of 25:1. Reports of cases in children have been associated with diaper use, excessive washing, and use of topical zinc oxide. It occurs in all races and ethnicities.
The condition was originally thought to occur solely in the axillae (previously known as axillary granular parakeratosis), but it is now recognized that GP can involve other intertriginous areas as well, such as the inframammary folds, abdominal folds, groin, and neck.
GP typically presents as reddish-brown, violaceous, or hyperpigmented scaly papules and plaques in intertriginous regions. Lesions can be asymptomatic or pruritic and friable.
GP is most commonly caused by heat, moisture, and friction. Axillary cases are hypothesized to be due to an irritant or allergic contact dermatitis due to a component of an antiperspirant.
GP has a relatively chronic course and can persist for several months or can resolve spontaneously, but recurrence is common.
Codes
L85.8 – Other specified epidermal thickening
SNOMEDCT:
56585003 – Parakeratosis of skin
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/03/2022