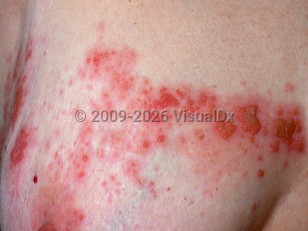
Herpes zoster - Oral Mucosal Lesion
See also in: Overview,Cellulitis DDx,Anogenital,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

Oral findings of zoster may be secondary to involvement of the maxillary or mandibular branch of the trigeminal nerve (V2 or V3 respectively). Intraoral zoster may be preceded by facial pain, toothache, or intraoral tingling. The upper cutaneous lip, palate, and upper gingiva may manifest grouped vesicles, which rupture rapidly if intraoral, eventuating into erosions. The remainder of the V2 dermatome, including the cheek and temple, may also be involved. In V3 zoster, the tongue, lower gingiva, buccal mucosa, floor of the mouth, and the lower cutaneous lip may be affected. Cutaneous involvement of V3 includes the chin, lower cheek over the mandible, preauricular area, and temporal scalp. With oral involvement, complete loss of or altered taste may occur.
Ramsay-Hunt syndrome occurs when VZV affects the geniculate ganglion of the facial nerve, typically giving rise to ipsilateral facial weakness, ear pain, vesicles of the external auditory canal and other parts of the ear, and hearing loss. The trigeminal nerve may be affected in this syndrome, in which case, the anterior two-thirds of the tongue, the palate, and/or the lips may be involved.
Herpes zoster duplex is the simultaneous occurrence of zoster in 2 noncontiguous dermatomes, and herpes zoster multiplex refers to this phenomenon occurring in more than 2 dermatomes. Disseminated zoster, defined as more than 20 vesicles outside of the primary and adjacent dermatomes, is chiefly a problem of immunocompromised patients (patients with HIV, patients with cancer, and those on immunosuppressive drugs). Some patients may suffer acute segmental neuralgia, known as zoster sine herpete, without ever developing a visible skin eruption. Regional adenopathy may be seen.
Zoster may be accompanied by pain acutely. Additionally, a major concern after a zoster outbreak is postherpetic neuralgia, defined as pain and neuropathic symptoms that persist in a dermatome one month beyond resolution of the rash. Risk factors for postherpetic neuralgia include older age, female sex, presence of a prodrome, greater rash severity, and acute pain. Postherpetic neuralgia can be intractable and debilitating, and prevention is an important goal. Other less frequently encountered post-zoster sequelae include herpes zoster granulomatous dermatitis (where a granulomatous eruption develops weeks to months after zoster resolution) and skin infiltration of the site of healed zoster by cells from an underlying hematologic malignancy (so-called isotopic response).
Cerebrovascular accidents, peripheral motor neuropathies, neurogenic bladder, and diaphragmatic paralysis have been associated with zoster. Herpes zoster encephalitis usually appears in the first 2 weeks after the onset of lesions and it has a 10%-20% mortality rate. Lesions may also be at risk for bacterial superinfection. In extreme cases, necrotizing fasciitis may occur. In the mouth, complications include periodontal inflammation, osteonecrosis, and loss of teeth.
Immunocompromised patient considerations: Immunocompromised patients have a higher risk of disseminated zoster. In patients with HIV and AIDS, multidermatomal, necrotic, or recurrent zoster may occur. Persistent ulcers and chronic hyperkeratotic zoster are further manifestations. A strong association of herpes zoster multiplex with underlying malignancy (especially lymphoma) was reported in one retrospective study. Osteonecrosis and associated loss of teeth are reported to occur more frequently in HIV-infected individuals.
Codes
B02.9 – Zoster without complications
SNOMEDCT:
4740000 – Herpes zoster
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:09/18/2024
 Patient Information for Herpes zoster - Oral Mucosal Lesion
Patient Information for Herpes zoster - Oral Mucosal Lesion- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient