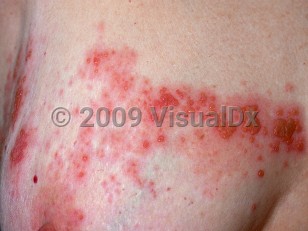
Herpes zoster in Adult
See also in: Cellulitis DDx,Anogenital,Hair and Scalp,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Cutaneous herpes zoster usually begins with a 1- to 3-day prodrome of burning pain or paresthesias in the affected dermatome, followed by eruption of erythematous papules and vesicles in the same distribution.
Involvement of a thoracic dermatome may simulate acute myocardial infarction. Involvement of the ophthalmic branch of the trigeminal nerve may lead to herpes zoster ophthalmicus. Herpes zoster oticus (Ramsay-Hunt syndrome) occurs with involvement of the vestibulocochlear nerve. Herpes zoster duplex is the simultaneous occurrence of zoster in 2 noncontiguous dermatomes, and herpes zoster multiplex refers to this phenomenon occurring in more than 2 dermatomes. Disseminated zoster, defined as more than 20 vesicles outside of the primary and adjacent dermatomes, is chiefly a problem of immunocompromised patients (patients with HIV, patients with cancer, and those on immunosuppressive drugs). Some patients may suffer acute segmental neuralgia, known as zoster sine herpete, without ever developing a visible skin eruption. Regional adenopathy may be seen.
Zoster may be accompanied by pain acutely. Additionally, a major concern after a zoster outbreak is postherpetic neuralgia, defined as pain and neuropathic symptoms that persist in a dermatome one month beyond resolution of the rash. Risk factors for postherpetic neuralgia include older age, female sex, presence of a prodrome, greater rash severity, and acute pain. Postherpetic neuralgia can be intractable and debilitating, and prevention is an important goal. Other less frequently encountered post-zoster sequelae include herpes zoster granulomatous dermatitis (where a granulomatous eruption develops weeks to months after zoster resolution) and skin infiltration of the site of healed zoster by cells from an underlying hematologic malignancy (so-called isotopic response).
Cerebrovascular accidents, peripheral motor neuropathies, neurogenic bladder, and diaphragmatic paralysis have been associated with zoster. Postherpetic abdominal pseudohernia refers to the abdominal asymmetry that is secondary to a motor neuropathy following zoster of a lower thoracic or lumbar dermatome. Herpes zoster encephalitis usually appears in the first 2 weeks after the onset of lesions, and it has a 10%-20% mortality rate. Lesions may also be at risk for bacterial superinfection. In extreme cases, necrotizing fasciitis may occur.
Immunocompromised patient considerations: Immunocompromised patients have a higher risk of disseminated zoster. In patients with HIV and AIDS, multidermatomal, necrotic, or recurrent zoster may occur. Persistent ulcers and chronic hyperkeratotic zoster are further manifestations. A strong association of herpes zoster multiplex with underlying malignancy (especially lymphoma) was reported in one retrospective study.
Codes
B02.9 – Zoster without complications
SNOMEDCT:
4740000 – Herpes zoster
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/28/2022
 Patient Information for Herpes zoster in Adult
Patient Information for Herpes zoster in Adult- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient