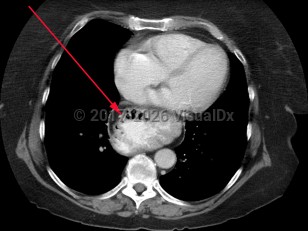
Hiatal hernias are typically asymptomatic. On occasion, patients will complain of vague abdominal discomfort. However, in most instances, they are diagnosed incidentally on cross-sectional imaging or upper endoscopy.
Hiatal hernias are classified as sliding or paraesophageal:
- Type I: sliding hernia – Most common type, due to progressive weakening of the gastroesophageal junction allowing a portion of the gastric cardia to slide upward with increased abdominal pressure, swallowing, and respiration. Patients with type I hernias are more likely to have gastroesophageal reflux disease (GERD).
- Types II, III, IV: paraesophageal hernia – Herniation includes viscera other than the gastric cardia, including gastric fundus and the colon. In type II and III hernias, the stomach becomes "inverted," possibly leading to gastric volvulus.