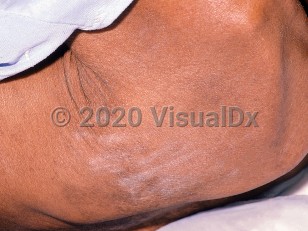
HIV/AIDS-related pruritus
Alerts and Notices
Important News & Links
Synopsis

Pruritus is a common problem in patients with human immunodeficiency virus (HIV) or acquired immune deficiency syndrome (AIDS). The itch can result from primary HIV-associated rashes, such as pruritic papular eruption and eosinophilic folliculitis, or it can accompany underlying skin conditions such as seborrheic dermatitis, photodermatitis, psoriasis, and atopic dermatitis. Pruritus can also reflect undiagnosed systemic disease or be idiopathic in up to 50% of patients, resulting in severe, chronic, and difficult to control symptoms.
Severe pruritus can occur either in patients who are well-controlled on antiviral therapy or in HIV-infected patients who are not on therapy. Treatment of pruritus should be guided by the primary morphology of the rash or lack thereof. A multiprong approach to treatment may be helpful as underlying dermatoses can be implicated. Idiopathic pruritus should be a diagnosis of exclusion.
Idiopathic, treatment-resistant pruritus is hypothesized to be secondary to the dysregulation of the immune response, which includes hyperactivation of the humoral response in HIV-infected patients. Eosinophilia and/or high IgE levels are sometimes present.
Related topics: pruritus without rash, xerosis
Severe pruritus can occur either in patients who are well-controlled on antiviral therapy or in HIV-infected patients who are not on therapy. Treatment of pruritus should be guided by the primary morphology of the rash or lack thereof. A multiprong approach to treatment may be helpful as underlying dermatoses can be implicated. Idiopathic pruritus should be a diagnosis of exclusion.
Idiopathic, treatment-resistant pruritus is hypothesized to be secondary to the dysregulation of the immune response, which includes hyperactivation of the humoral response in HIV-infected patients. Eosinophilia and/or high IgE levels are sometimes present.
Related topics: pruritus without rash, xerosis
Codes
ICD10CM:
L29.8 – Other pruritus
SNOMEDCT:
420721002 – AIDS-associated disorder
L29.8 – Other pruritus
SNOMEDCT:
420721002 – AIDS-associated disorder
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:01/03/2018
Last Updated:01/16/2020
Last Updated:01/16/2020