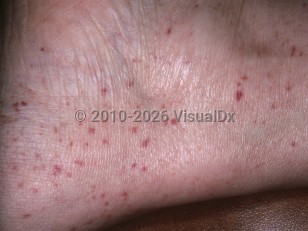
Hyperglobulinemic purpura of Waldenström
Alerts and Notices
Important News & Links
Synopsis

Hyperglobulinemic purpura of Waldenström is a rare chronic disorder characterized by recurrent crops of nonthrombocytopenic petechiae and purpura on the dependent areas of the body, polyclonal hypergammaglobulinemia, and elevated ESR. This condition most commonly affects young to middle-aged females (late teens to 40s) but can be seen in children.
Hyperglobulinemic purpura of Waldenström is classified as primary (idiopathic) or secondary to an underlying disease. Associated diseases include autoimmune connective tissue disorders, most commonly Sjögren syndrome; occasionally systemic lupus erythematosus, rheumatoid arthritis, autoimmune hepatitis, hepatitis C, or cystic fibrosis; and rarely hematologic malignancies, such as monoclonal gammopathy, lymphoma, or multiple myeloma. The onset of hypergammaglobulinemic purpura often precedes the underlying disease by many years, with some associated diseases developing 10 or more years later. Autoantibodies that are commonly positive include Ro/SS-A, La/SS-B, antinuclear antibodies (ANA), and rheumatoid factor (RF). The presence of anti-Ro/SS-A and anti-La/SS-B antibodies may predict a higher likelihood of developing an associated autoimmune connective tissue disorder. Mild anemia or lymphopenia can also be found.
The petechiae and purpura are frequently exacerbated by prolonged periods of standing, wearing tight clothing, alcohol intake, and exercise. The eruption is usually asymptomatic, yet some patients may report burning, stinging, pruritus, or lower extremity swelling. The pathogenesis of purpura is thought to be due to immune complex deposition in the blood vessels of the lower extremities. Truncal involvement can also be seen.
When this condition is seen in pregnancy, it is not considered benign; all reported cases are associated with anti-SS-A antibodies, with potential increased risk of poor maternal / fetal outcome including intrauterine fetal growth restriction, congenital heart block, and fetal demise. More than half of children, as reported in the literature, will go on to develop an autoimmune condition.
Hyperglobulinemic purpura of Waldenström is classified as primary (idiopathic) or secondary to an underlying disease. Associated diseases include autoimmune connective tissue disorders, most commonly Sjögren syndrome; occasionally systemic lupus erythematosus, rheumatoid arthritis, autoimmune hepatitis, hepatitis C, or cystic fibrosis; and rarely hematologic malignancies, such as monoclonal gammopathy, lymphoma, or multiple myeloma. The onset of hypergammaglobulinemic purpura often precedes the underlying disease by many years, with some associated diseases developing 10 or more years later. Autoantibodies that are commonly positive include Ro/SS-A, La/SS-B, antinuclear antibodies (ANA), and rheumatoid factor (RF). The presence of anti-Ro/SS-A and anti-La/SS-B antibodies may predict a higher likelihood of developing an associated autoimmune connective tissue disorder. Mild anemia or lymphopenia can also be found.
The petechiae and purpura are frequently exacerbated by prolonged periods of standing, wearing tight clothing, alcohol intake, and exercise. The eruption is usually asymptomatic, yet some patients may report burning, stinging, pruritus, or lower extremity swelling. The pathogenesis of purpura is thought to be due to immune complex deposition in the blood vessels of the lower extremities. Truncal involvement can also be seen.
When this condition is seen in pregnancy, it is not considered benign; all reported cases are associated with anti-SS-A antibodies, with potential increased risk of poor maternal / fetal outcome including intrauterine fetal growth restriction, congenital heart block, and fetal demise. More than half of children, as reported in the literature, will go on to develop an autoimmune condition.
Codes
ICD10CM:
D89.0 – Polyclonal hypergammaglobulinemia
SNOMEDCT:
190809001 – Waldenstrom hypergammaglobulinemic purpura
D89.0 – Polyclonal hypergammaglobulinemia
SNOMEDCT:
190809001 – Waldenstrom hypergammaglobulinemic purpura
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:12/16/2020
Last Updated:12/16/2020
Last Updated:12/16/2020
Hyperglobulinemic purpura of Waldenström