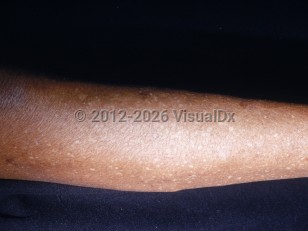
Idiopathic guttate hypomelanosis
Alerts and Notices
Important News & Links
Synopsis

Idiopathic guttate hypomelanosis (IGH) is a common acquired condition, characterized by scattered 3- to 5-mm hypopigmented macules occurring on chronically sun-exposed skin. IGH typically occurs in middle-aged individuals with photodamage and increases in incidence with age and continued sun exposure.
While the exact cause is unknown, IGH has been hypothesized to be ultraviolet (UV) induced. Other contributing factors that have been suggested include aging, trauma, genetic factors, and autoimmunity.
While IGH occurs more commonly in lighter skin phototypes, it does occur in all skin colors, and it appears more prominent in individuals with darker skin.
While the exact cause is unknown, IGH has been hypothesized to be ultraviolet (UV) induced. Other contributing factors that have been suggested include aging, trauma, genetic factors, and autoimmunity.
While IGH occurs more commonly in lighter skin phototypes, it does occur in all skin colors, and it appears more prominent in individuals with darker skin.
Codes
ICD10CM:
L81.9 – Disorder of pigmentation, unspecified
SNOMEDCT:
1717003 – Idiopathic guttate hypomelanosis
L81.9 – Disorder of pigmentation, unspecified
SNOMEDCT:
1717003 – Idiopathic guttate hypomelanosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:03/18/2020
Last Updated:03/22/2021
Last Updated:03/22/2021
 Patient Information for Idiopathic guttate hypomelanosis
Patient Information for Idiopathic guttate hypomelanosis
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Idiopathic guttate hypomelanosis