Emergency: requires immediate attention
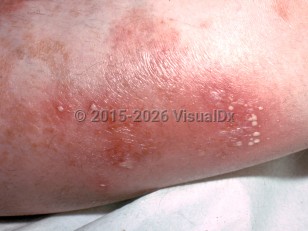
Pustular psoriasis of pregnancy
Alerts and Notices
Important News & Links
Synopsis

Pustular psoriasis of pregnancy (PPP), also known as impetigo herpetiformis, is a rare pustular dermatosis typically seen in the third trimester of pregnancy. The exact prevalence is unknown, but there have been fewer than 200 reported cases to date.
It is unclear whether PPP is a separate entity from generalized pustular psoriasis (GPP). Many women who develop PPP have no personal or family history of psoriasis. Some women with biopsy-proven pustular psoriasis in pregnancy subsequently develop GPP later in life.
Pathogenesis is poorly understood, but it may be related to the increase in progesterone in late pregnancy. PPP can also arise during menstrual cycles and affect patients taking oral contraceptive pills, further supporting a role of hormones in pathogenesis. Some authors relate PPP to the hypocalcemia that may develop in late pregnancy due to volume expansion and increased renal clearance, and hypocalcemia and low vitamin D can be seen in PPP in the absence of pregnancy. PPP is also sometimes accompanied by hypoparathyroidism. Drug-induced cases have been reported in patients taking ritodrine hydrochloride, which has been used to suppress preterm uterine contractions.
The eruption usually begins in the third trimester of pregnancy (after 26 weeks) but may occur at any time during pregnancy. It commonly recurs in subsequent pregnancies, typically with earlier onset and greater severity with each successive pregnancy. It may be accompanied by systemic symptoms and signs including fever, chills, nausea, vomiting, diarrhea, malaise, and lymphadenopathy. Further maternal complications include electrolyte imbalance, fluid loss, and sepsis from secondary infection. Hypocalcemia can result in delirium, tetany, and convulsions. Fetal complications include placental insufficiency, intrauterine fetal demise, neonatal death, and low birth weight.
It is unclear whether PPP is a separate entity from generalized pustular psoriasis (GPP). Many women who develop PPP have no personal or family history of psoriasis. Some women with biopsy-proven pustular psoriasis in pregnancy subsequently develop GPP later in life.
Pathogenesis is poorly understood, but it may be related to the increase in progesterone in late pregnancy. PPP can also arise during menstrual cycles and affect patients taking oral contraceptive pills, further supporting a role of hormones in pathogenesis. Some authors relate PPP to the hypocalcemia that may develop in late pregnancy due to volume expansion and increased renal clearance, and hypocalcemia and low vitamin D can be seen in PPP in the absence of pregnancy. PPP is also sometimes accompanied by hypoparathyroidism. Drug-induced cases have been reported in patients taking ritodrine hydrochloride, which has been used to suppress preterm uterine contractions.
The eruption usually begins in the third trimester of pregnancy (after 26 weeks) but may occur at any time during pregnancy. It commonly recurs in subsequent pregnancies, typically with earlier onset and greater severity with each successive pregnancy. It may be accompanied by systemic symptoms and signs including fever, chills, nausea, vomiting, diarrhea, malaise, and lymphadenopathy. Further maternal complications include electrolyte imbalance, fluid loss, and sepsis from secondary infection. Hypocalcemia can result in delirium, tetany, and convulsions. Fetal complications include placental insufficiency, intrauterine fetal demise, neonatal death, and low birth weight.
Codes
ICD10CM:
L40.1 – Generalized pustular psoriasis
SNOMEDCT:
238613007 – Generalized pustular psoriasis of pregnancy
L40.1 – Generalized pustular psoriasis
SNOMEDCT:
238613007 – Generalized pustular psoriasis of pregnancy
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/24/2023
Last Updated:09/21/2025
Last Updated:09/21/2025
Emergency: requires immediate attention
Pustular psoriasis of pregnancy