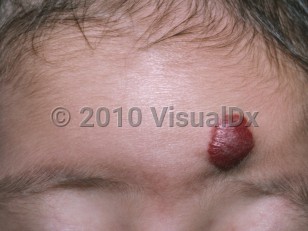
Infantile hemangioma in Child
See also in: External and Internal Eye,AnogenitalAlerts and Notices
Important News & Links
Synopsis

Infantile hemangiomas are the most common benign tumors of infancy, occurring in up to 10% of infants, with up to 50% involving the head and neck. Precursors may be present at birth, evolving into a more classic appearance within the first few months of life. Usually, infantile hemangiomas grow rapidly during the first few weeks of life. This initial proliferative phase typically peaks as early as 2 months of age. This is followed by a steady state lasting months, depending on the hemangioma type, followed by gradual involution over several years, with more than 90% completely involuting by age 10. Although infantile hemangiomas involute with time, residual skin changes such as telangiectasia, scarring, atrophy, and fibrosis persist in up to 30% of lesions after involution is complete.
Ulceration occurs in about 5% of hemangiomas and can occur at any location. Ulcerated hemangiomas are painful regardless of location, often become secondarily infected, and leave a scar. Bleeding and ulceration can incorrectly cause or increase concern for possible physical abuse; however, their characteristic development in early infancy and typical regression should help differentiate them from the former. Ulceration is of particular concern when it involves the periocular, nasal, perioral, or anogenital areas, given regional risk for severe complication. Ulceration of the nasal or laryngeal areas can cause respiratory compromise. Perioral ulceration can interfere with latching and feeding. Anogenital ulceration adversely affects diaper changes, urination, and defecation. Periocular ulceration and attendant scarring can distort the eyelids, scar the cornea, and/or affect development of binocular vision. Only about 1%-2% of hemangiomas involve the genitalia. Such hemangiomas of the urethra, the labia, hymen, vulva, or perihymenal area may raise concern for sexual abuse. When extensive ulceration is present, there may be concern that these represent perineal burns. Knowledge of the clinical appearance and natural course of untreated hemangiomas may help prevent misdiagnosis.
Segmental infantile hemangiomas raise concern for regional abnormalities. A segmental infantile hemangioma of the upper face, ears, and/or scalp requires evaluation for PHACE syndrome (posterior fossa anomalies, hemangioma, arterial anomalies, cardiac anomalies, and eye anomalies). Involvement of the lower face and neck warrant assessment for laryngeal involvement. If the anogenital area is involved in a segmental fashion, evaluation for associated anomalies associated with the synonymous LUMBAR syndrome (lower body hemangioma, lipoma, or other cutaneous anomalies, urogenital anomalies, myelopathy, bony deformities, anorectal and arterial anomalies, and renal anomalies), SACRAL syndrome (spinal dysraphism, anogenital anomalies, cutaneous anomalies, renal and urologic anomalies, associated with angioma of lumbosacral localization), or PELVIS syndrome (perineal hemangioma, external genitalia malformations, lipomyelomeningocele, vesicorenal abnormalities, imperforate anus, and skin tags) should ensue.
Ulceration occurs in about 5% of hemangiomas and can occur at any location. Ulcerated hemangiomas are painful regardless of location, often become secondarily infected, and leave a scar. Bleeding and ulceration can incorrectly cause or increase concern for possible physical abuse; however, their characteristic development in early infancy and typical regression should help differentiate them from the former. Ulceration is of particular concern when it involves the periocular, nasal, perioral, or anogenital areas, given regional risk for severe complication. Ulceration of the nasal or laryngeal areas can cause respiratory compromise. Perioral ulceration can interfere with latching and feeding. Anogenital ulceration adversely affects diaper changes, urination, and defecation. Periocular ulceration and attendant scarring can distort the eyelids, scar the cornea, and/or affect development of binocular vision. Only about 1%-2% of hemangiomas involve the genitalia. Such hemangiomas of the urethra, the labia, hymen, vulva, or perihymenal area may raise concern for sexual abuse. When extensive ulceration is present, there may be concern that these represent perineal burns. Knowledge of the clinical appearance and natural course of untreated hemangiomas may help prevent misdiagnosis.
Segmental infantile hemangiomas raise concern for regional abnormalities. A segmental infantile hemangioma of the upper face, ears, and/or scalp requires evaluation for PHACE syndrome (posterior fossa anomalies, hemangioma, arterial anomalies, cardiac anomalies, and eye anomalies). Involvement of the lower face and neck warrant assessment for laryngeal involvement. If the anogenital area is involved in a segmental fashion, evaluation for associated anomalies associated with the synonymous LUMBAR syndrome (lower body hemangioma, lipoma, or other cutaneous anomalies, urogenital anomalies, myelopathy, bony deformities, anorectal and arterial anomalies, and renal anomalies), SACRAL syndrome (spinal dysraphism, anogenital anomalies, cutaneous anomalies, renal and urologic anomalies, associated with angioma of lumbosacral localization), or PELVIS syndrome (perineal hemangioma, external genitalia malformations, lipomyelomeningocele, vesicorenal abnormalities, imperforate anus, and skin tags) should ensue.
Codes
ICD10CM:
D18.01 – Hemangioma of skin and subcutaneous tissue
SNOMEDCT:
83343001 – Infantile hemangioma
D18.01 – Hemangioma of skin and subcutaneous tissue
SNOMEDCT:
83343001 – Infantile hemangioma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/06/2021
Last Updated:01/17/2022
Last Updated:01/17/2022
 Patient Information for Infantile hemangioma in Child
Patient Information for Infantile hemangioma in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Infantile hemangioma in Child
See also in: External and Internal Eye,Anogenital