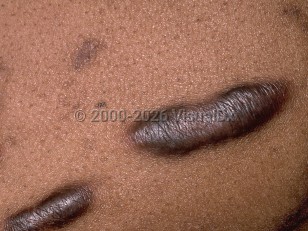
Keloid in Child
Alerts and Notices
Important News & Links
Synopsis

Keloids are dense, fibrotic papules, plaques, or nodules found at areas of previously traumatized skin (eg, burns, lacerations, incision scars) or arising spontaneously on normal skin.
Keloids may be single or multiple. They may be painful, tender, pruritic, and can grow to become very large (up to 30 cm). They can cause chronic discomfort, be disfiguring, and restrict normal tissue motion.
Keloids can affect individuals of any race and ethnicity. There is likely a genetic basis for the tendency to develop keloids, and research is ongoing. Most susceptible individuals start developing keloids in their 20s. Keloid formation is associated with hypertension and obesity.
Keloids may be single or multiple. They may be painful, tender, pruritic, and can grow to become very large (up to 30 cm). They can cause chronic discomfort, be disfiguring, and restrict normal tissue motion.
Keloids can affect individuals of any race and ethnicity. There is likely a genetic basis for the tendency to develop keloids, and research is ongoing. Most susceptible individuals start developing keloids in their 20s. Keloid formation is associated with hypertension and obesity.
Codes
ICD10CM:
L91.0 – Hypertrophic scar
SNOMEDCT:
33659008 – Keloid scar
L91.0 – Hypertrophic scar
SNOMEDCT:
33659008 – Keloid scar
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/12/2024
Last Updated:10/13/2024
Last Updated:10/13/2024
 Patient Information for Keloid in Child
Patient Information for Keloid in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Keloid in Child