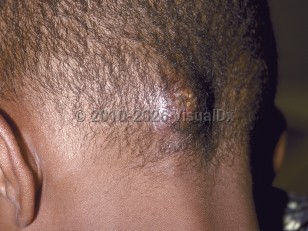
Kerion in Infant/Neonate
See also in: Cellulitis DDx,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

A kerion is an acute inflammatory reaction that accompanies severe cases of tinea capitis (also known as ringworm of the scalp) and tinea barbae (also known as ringworm of the beard). Kerions may involve other hairbearing sites such as the eyebrows and vulva. Kerions are often caused by an organism from an animal or the soil, such as Trichophyton verrucosum, Trichophyton tonsurans, or Microsporum canis. New pathogens, such as Trichophyton Arthroderma benhamiae, have been identified.
A kerion will occur in a patient who has an intact immune response and develops an intense inflammatory response to the organisms. It is almost exclusively seen in children, but on rare occasions, it may be seen in adolescents and young adults. As in tinea capitis, this disease is more common in patients of African descent. It is more common in males than females and in those with short hair. Other risk factors include diabetes, anemia, immunosuppression, underlying malignancy, and organ transplantation. It is seen less frequently in HIV-infected patients; this may be due to increased colonization with Malassezia, which may inhibit dermatophyte colonization.
Fever, pain, occipital lymphadenopathy, and secondary bacterial infection may be associated. The intensity of the inflammation depends on the host immune response. If left untreated, scarring and permanent alopecia can develop. Patients with kerion may develop immunological dermatophytid reactions, which may be localized or generalized. The "ear sign" is a dermatophytid reaction that presents as erythematous plaques and papules on the helix, antihelix, and retroauricular region.
Kerions can be distinguished from cellulitis based on their location and the presence of other signs of a fungal infection, such as scaling.
A kerion will occur in a patient who has an intact immune response and develops an intense inflammatory response to the organisms. It is almost exclusively seen in children, but on rare occasions, it may be seen in adolescents and young adults. As in tinea capitis, this disease is more common in patients of African descent. It is more common in males than females and in those with short hair. Other risk factors include diabetes, anemia, immunosuppression, underlying malignancy, and organ transplantation. It is seen less frequently in HIV-infected patients; this may be due to increased colonization with Malassezia, which may inhibit dermatophyte colonization.
Fever, pain, occipital lymphadenopathy, and secondary bacterial infection may be associated. The intensity of the inflammation depends on the host immune response. If left untreated, scarring and permanent alopecia can develop. Patients with kerion may develop immunological dermatophytid reactions, which may be localized or generalized. The "ear sign" is a dermatophytid reaction that presents as erythematous plaques and papules on the helix, antihelix, and retroauricular region.
Kerions can be distinguished from cellulitis based on their location and the presence of other signs of a fungal infection, such as scaling.
Codes
ICD10CM:
B35.0 – Tinea barbae and tinea capitis
SNOMEDCT:
19087001 – Kerion
B35.0 – Tinea barbae and tinea capitis
SNOMEDCT:
19087001 – Kerion
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:04/02/2019
Last Updated:05/05/2019
Last Updated:05/05/2019
 Patient Information for Kerion in Infant/Neonate
Patient Information for Kerion in Infant/Neonate
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Kerion in Infant/Neonate
See also in: Cellulitis DDx,Hair and Scalp