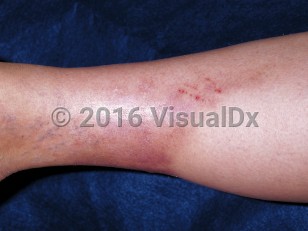
Lipodermatosclerosis
Alerts and Notices
Important News & Links
Synopsis

In the United States, 6%-7% of the population aged older than 50 years has some form of chronic venous insufficiency. The incidence peaks in women aged 40-50 years and men aged 70-79 years. Risk factors include age, smoking, family history, preexisting varicose veins, previous trauma to the venous system (eg, vein stripping, nonsurgical trauma), hypercoagulable states (eg, protein C or S deficiency), history of deep vein thrombosis, obesity, and lifestyle choices (eg, standing occupations, sedentary lifestyle). Clinical features of chronic venous stasis include varicose veins, lower extremity edema, chronic aching pain from venous hypertension of muscle and fascial compartments, and, finally, progression to lipodermatosclerosis and the development of nonhealing ulcers.
The exact pathogenesis of lipodermatosclerosis is unknown. It is believed that venous disease (ie, venous hypertension, venous incompetence, etc) allows diffusion of capillary contents such as fibrinogen and other inflammatory mediators into the dermis. Fibrinogen is polymerized to fibrin, which forms a fibrin cuff around capillaries, leading to a relative hypoxic state. This is complicated by elevated proteolytic activity involving matrix metalloproteinases and fibrinolytic mediators from the plasminogen activating pathway, which degrades the collagen matrix, resulting in venous ulcers.
Codes
I83.10 – Varicose veins of unspecified lower extremity with inflammation
SNOMEDCT:
410016009 – Lipodermatosclerosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:01/31/2021